Key Takeaways
- Thyroid cancer is highly treatable, especially when found early.
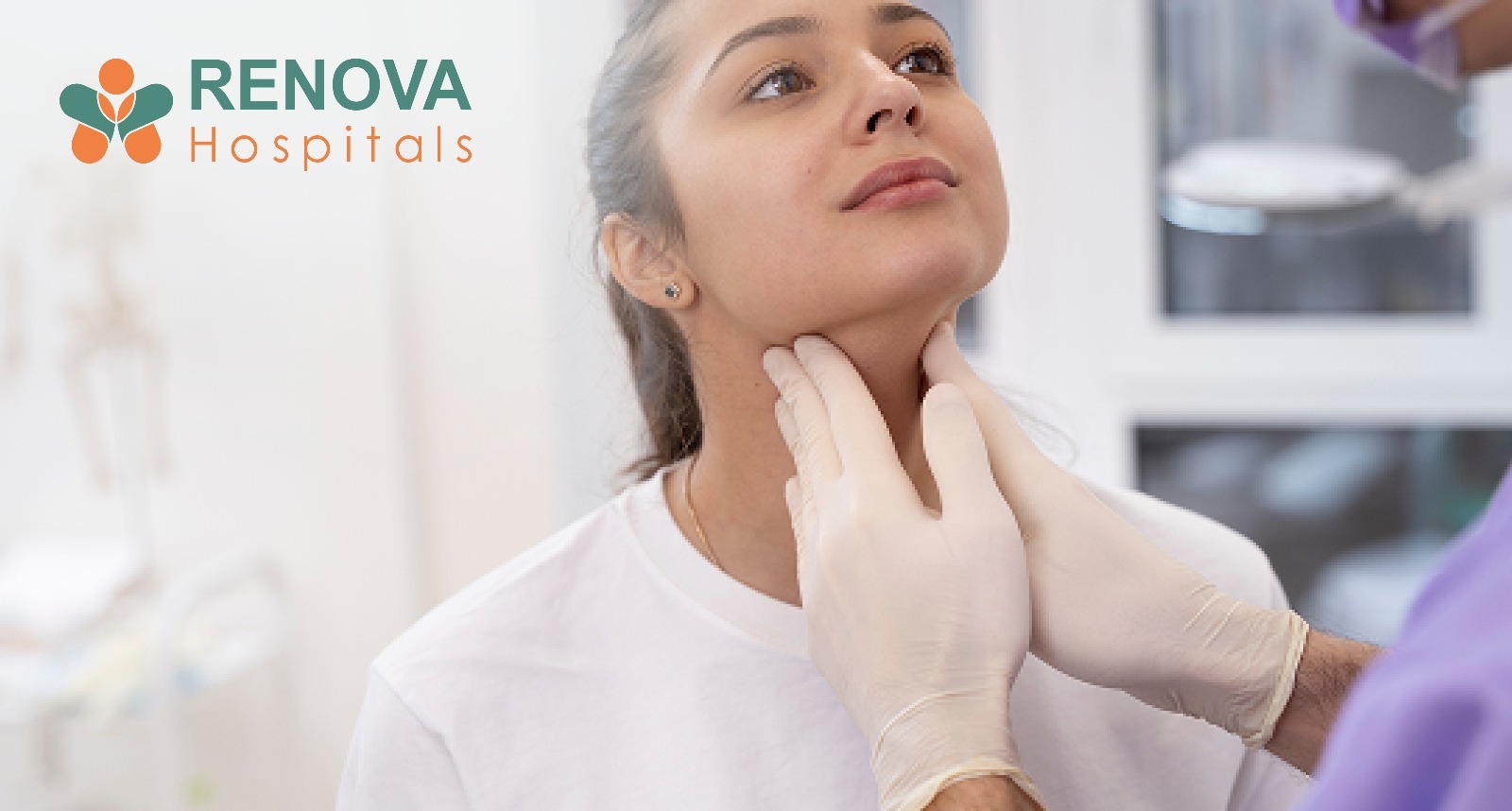
- A painless neck lump is the most common early sign.
- Women are at higher risk, and cases are rising in young adults.
- Ultrasound and biopsy confirm the diagnosis.
- Surgery is the main treatment, sometimes followed by radioactive iodine.
- Early detection leads to excellent survival and normal life expectancy.
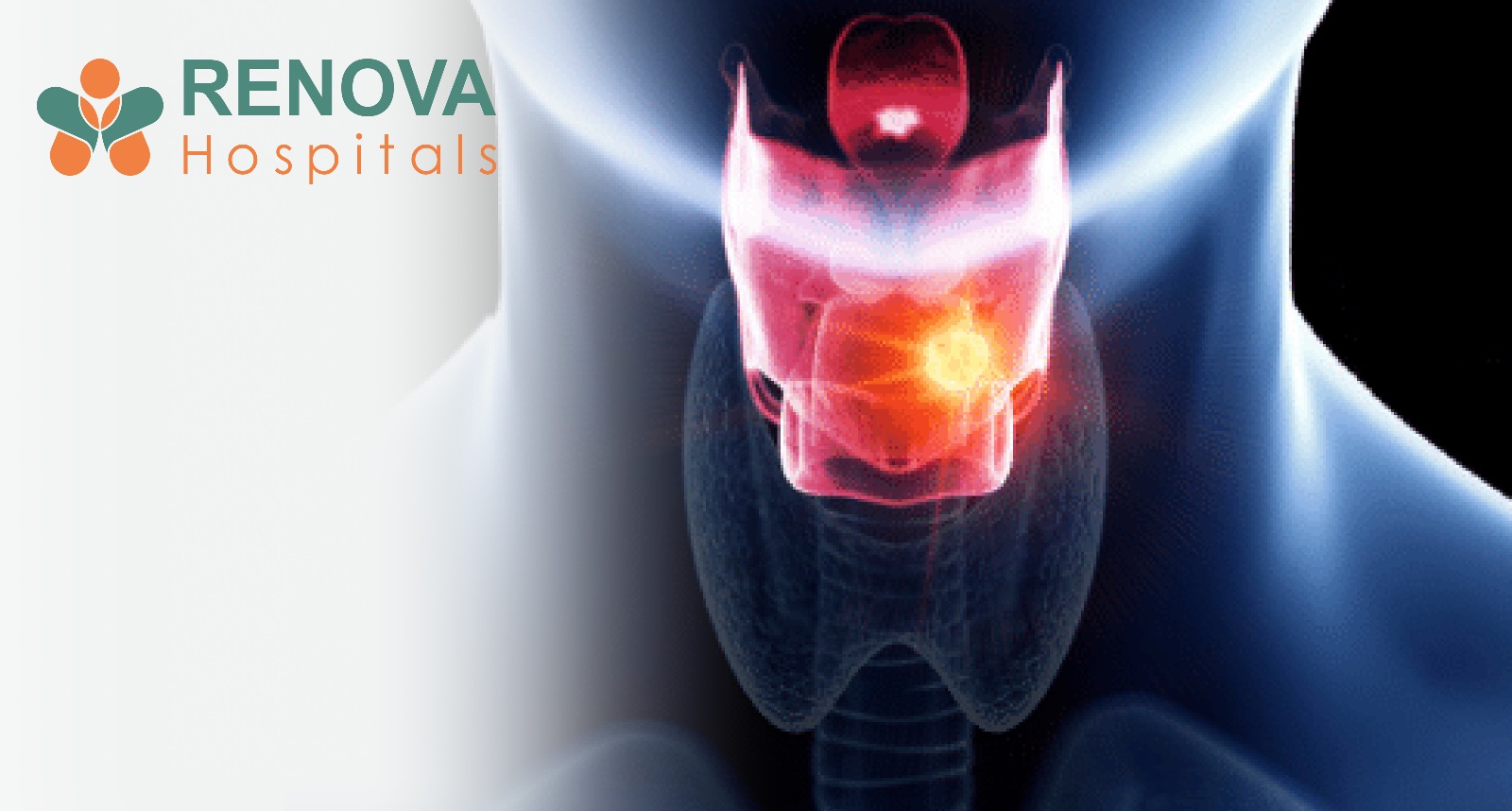
What Is Thyroid Cancer?
Your thyroid is a small, butterfly-shaped gland at the base of your neck. It acts as your body’s control centre, managing:
- Metabolism
- Heart rate
- Body temperature
- Bone and muscle health
- Energy levels
Thyroid cancer happens when cells in the gland undergo changes and begin to grow into a tumour. Most thyroid cancers arise from follicular cells that produce hormones. In some cases, they are classified as differentiated thyroid
cancer, which includes papillary and follicular types. These cancers generally grow slowly and have an excellent prognosis when detected early.
Why Are We Seeing More Cases of Thyroid Cancer?
Over the past three decades, global thyroid cancer incidence has increased significantly. Research indicates:
- A substantial rise among individuals aged 15 to 39 years
- Higher incidence in women (nearly three times more than men)
- Increasing detection due to widespread ultrasound screening
- Regional disparities, with rising cases in South Asia and lower-income regions
Because our scanning technology has become so precise, we can now catch tiny nodules much earlier than before. However, environmental, hormonal, and lifestyle factors may also contribute.
Types of Thyroid Cancer
Thyroid cancers are classified based on how the cancer cells appear under a microscope and on their aggressiveness.
Papillary Thyroid Cancer
This is the most common type, accounting for approximately 80–85% of cases.
It typically:
- Grows slowly
- May spread to nearby lymph nodes
- Has an excellent prognosis
- Shows over 99% five-year survival when localised
Papillary thyroid cancer often affects younger women and is frequently detected during routine examinations.
Follicular Thyroid Cancer
The second most common type, representing about 10–15% of cases.
It:
- It is more common in iodine-deficient regions
- May spread to the lungs or bones
- Has a slightly more aggressive behaviour than papillary cancer
- Still maintains very high survival rates when detected early
Medullary Thyroid Cancer
This type arises from C-cells that produce calcitonin.
Key features include:
- May be hereditary (associated with MEN2 syndrome)
- Produces elevated calcitonin levels detectable in blood tests
- More aggressive than differentiated cancers
- Requires genetic evaluation in selected patients
Anaplastic Thyroid Cancer
A rare but highly aggressive form, accounting for less than 2% of cases.
It:
- Grows rapidly
- Spreads early
- Has a lower survival rate
- Requires urgent, multidisciplinary treatment
Hürthle Cell Carcinoma
A rare variant of follicular cancer that may be more resistant to radioactive iodine therapy.
Early Signs and Symptoms of Thyroid Cancer
Many patients do not experience symptoms in the early stages. Thyroid cancer is often detected incidentally during routine health check-ups.
Common Early Symptoms
- A painless lump in the neck
- Swollen lymph nodes
- Hoarseness or persistent voice changes
- Difficulty swallowing
- Persistent cough not related to infection
- Sensation of fullness in the throat
If you feel a lump, you’ll notice it feels much harder or 'fixed' compared to the soft tissue around it.
Symptoms of Advanced Thyroid Cancer
If the cancer spreads beyond the thyroid gland, patients may experience:
- Bone pain
- Shortness of breath
- Unintended weight loss
- Fatigue
- Persistent neck pain
Note: Having an overactive thyroid (hyperthyroidism) usually does not mean cancer is present, although some patients may have thyroid hormone imbalances.
Risk Factors for Thyroid Cancer
A combination of genetic, environmental, and hormonal factors influences thyroid cancer.
Established Risk Factors Include:
- Radiation exposure during childhood (the strongest risk factor)
- Female gender
- Age above 50 years
- Family history of thyroid cancer
- Genetic mutations such as BRAF and RET
- MEN2 syndrome
- Iodine deficiency
- Obesity
- Environmental pollutants
Hormonal fluctuations during puberty, pregnancy, and reproductive years may partly explain the higher incidence in women.
Thyroid Cancer in Young Adults (15–39 Years)
Recent global health studies show:
- A 150% increase in cases since 1990
- Highest growth in the 20–24 age group
- Higher incidence in females
- Projected continued rise in lower-income regions by 2050
Although mortality remains low, the disease burden in terms of treatment costs, psychological stress, and long-term monitoring is significant.
How Is Thyroid Cancer Diagnosed?
Getting an accurate diagnosis is the first and most vital step in building your recovery plan.
Clinical Examination
The doctor evaluates the neck for swelling, nodules, or enlarged lymph nodes.
Ultrasound Scan
Ultrasound helps identify suspicious nodules based on:
- Irregular borders
- Microcalcifications
- Increased vascularity
- Hypoechoic appearance
Fine Needle Aspiration (FNA) Biopsy
This is the gold standard diagnostic test. A thin needle is used to extract cells from the nodule for microscopic examination.
Blood Tests
Doctors may check:
- Thyroglobulin levels
- Calcitonin (for medullary thyroid cancer)
- TSH levels
Imaging for Staging
CT scans, PET scans, or radioactive iodine scans are performed if cancer spread is suspected.
At Renova Hospitals, we follow internationally accepted oncology guidelines to ensure accurate diagnosis and staging.mmhcj m
Staging of Thyroid Cancer
Thyroid cancer staging depends on:
- Tumour size
- Lymph node involvement
- Presence of distant metastasis
- Patient’s age
In the early stages, the cancer is confined to the thyroid gland. As stages advance, the tumour may extend locally, involve lymph nodes, or spread to distant organs such as lungs or bones.
Younger patients often have better stage-based outcomes compared to older individuals.
Treatment Options for Thyroid Cancer
Every patient is different; we tailor your treatment plan based on the specific type of cancer and your unique health needs.
Surgery
For most patients, the first and most effective step toward recovery is surgery.
Options include:
- Lobectomy (removal of one lobe)
- Total thyroidectomy (removal of entire gland)
- Lymph node dissection if required
Radioactive Iodine Therapy (RAI)
RAI is used after surgery in differentiated thyroid cancers to destroy the remaining thyroid tissue.
Thyroid Hormone Replacement Therapy
Patients who undergo total thyroidectomy require lifelong hormone replacement therapy.
Targeted Therapy
Advanced cancers with specific genetic mutations may benefit from targeted drugs such as BRAF or RET inhibitors.
Immunotherapy
Immunotherapy, particularly PD-1/PD-L1 inhibitors, is used in aggressive or anaplastic thyroid cancer.
Chemotherapy
Rarely used, reserved for selected advanced cases.
At Renova Hospitals, thyroid cancer treatment is delivered through a multidisciplinary team approach, ensuring personalised care and improved outcomes.
What is the Outlook? Understanding Survival Rates
Thyroid cancer has one of the highest survival rates among cancers. The outlook is exceptionally positive; nearly all patients with localised thyroid cancer go on to live full, healthy lives. Even when the disease spreads regionally, survival remains very high.
In cases of distant spread:
- Papillary thyroid cancer has around 74% five-year survival
- Follicular thyroid cancer has an approximately 67%
- Medullary thyroid cancer accounts for about 43%
- Anaplastic thyroid cancer is significantly lower, around 4%, in distant stages
Overall, the five-year
survival rate across all types exceeds 98%.
Is Thyroid Cancer Curable?
Yes. Most early-stage thyroid cancers are completely curable, particularly papillary and follicular types.
Even in advanced cases, modern targeted therapy and immunotherapy have significantly improved outcomes. Early detection is the single most important factor in ensuring a successful recovery and long-term health.
Quality of Life After Thyroid Cancer Treatment
Most of our patients get back to their normal daily routines and enjoy a high quality of life after treatment. However, some may experience:
- Fatigue
- Voice changes
- Hypothyroidism
- Emotional stress
- Need for lifelong follow-up
Lobectomy may preserve a better quality of life in selected patients compared to total thyroidectomy. Regular follow-up helps monitor hormone levels and detect recurrence early.
Prevention and Screening
Routine screening is not recommended for individuals without symptoms due to the risk of overdiagnosis.
High-risk individuals should undergo regular monitoring if they have:
- History of radiation exposure
- Strong family history
- Genetic predisposition
Lifestyle Measures
- Maintain adequate iodine intake
- Manage weight
- Avoid unnecessary radiation exposure
- Follow regular health check-ups
When Should You Consult a Specialist?
Seek medical attention if you notice:
- A persistent neck lump
- Voice changes lasting more than two weeks
- Difficulty swallowing
- Unexplained neck swelling
Early evaluation can significantly improve outcomes.
Expert Thyroid Cancer Care at Renova Hospitals
- Advanced diagnostic imaging
- Experienced surgical oncology specialists
- Personalised treatment planning
- Multidisciplinary tumour board discussions
- Comprehensive post-treatment follow-up
Our goal is not only to treat cancer but also to preserve quality of life and provide long-term reassurance. If you or a loved one is experiencing symptoms of thyroid cancer, timely consultation can make a significant difference.
Medical Disclaimer
This article is for educational purposes only and does not replace professional medical advice. For personalised diagnosis and treatment recommendations, consult a qualified oncologist or endocrinologist at Renova Hospitals.