By Renova hospitals
February 26, 2026
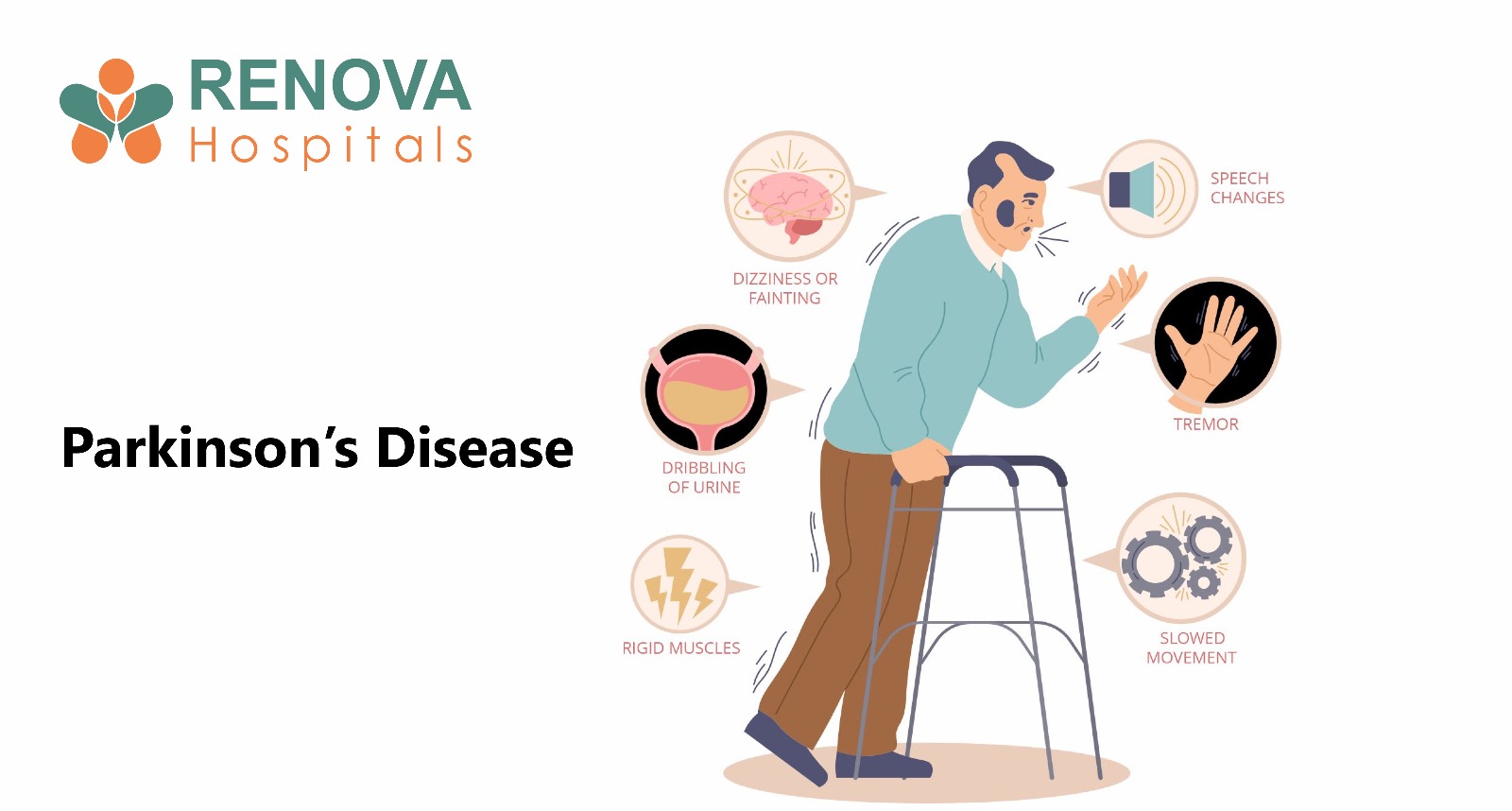
Parkinson’s Disease: Symptoms, Causes, Diagnosis & Advanced Treatment
What You Need to Know
- Parkinson’s disease is a progressive neurological disorder caused by dopamine deficiency in the brain.
- Early signs include resting tremor, slow movements, stiffness, and balance problems.
- Non-motor symptoms like depression, sleep disturbances, constipation, and memory issues are common.
- There is no cure, but Parkinson’s disease treatment with medications like carbidopa-levodopa significantly improves symptoms.
- Advanced options such as Deep Brain Stimulation (DBS) may help selected patients.
- Diet, physiotherapy, speech therapy, and regular exercise play an important role in long-term management.
- Early diagnosis by a neurologist improves quality of life and functional independence.
What Is Parkinson’s Disease?
- Movements become slower (bradykinesia)
- Muscles become stiff (rigidity)
- Tremors develop
- Balance becomes impaired
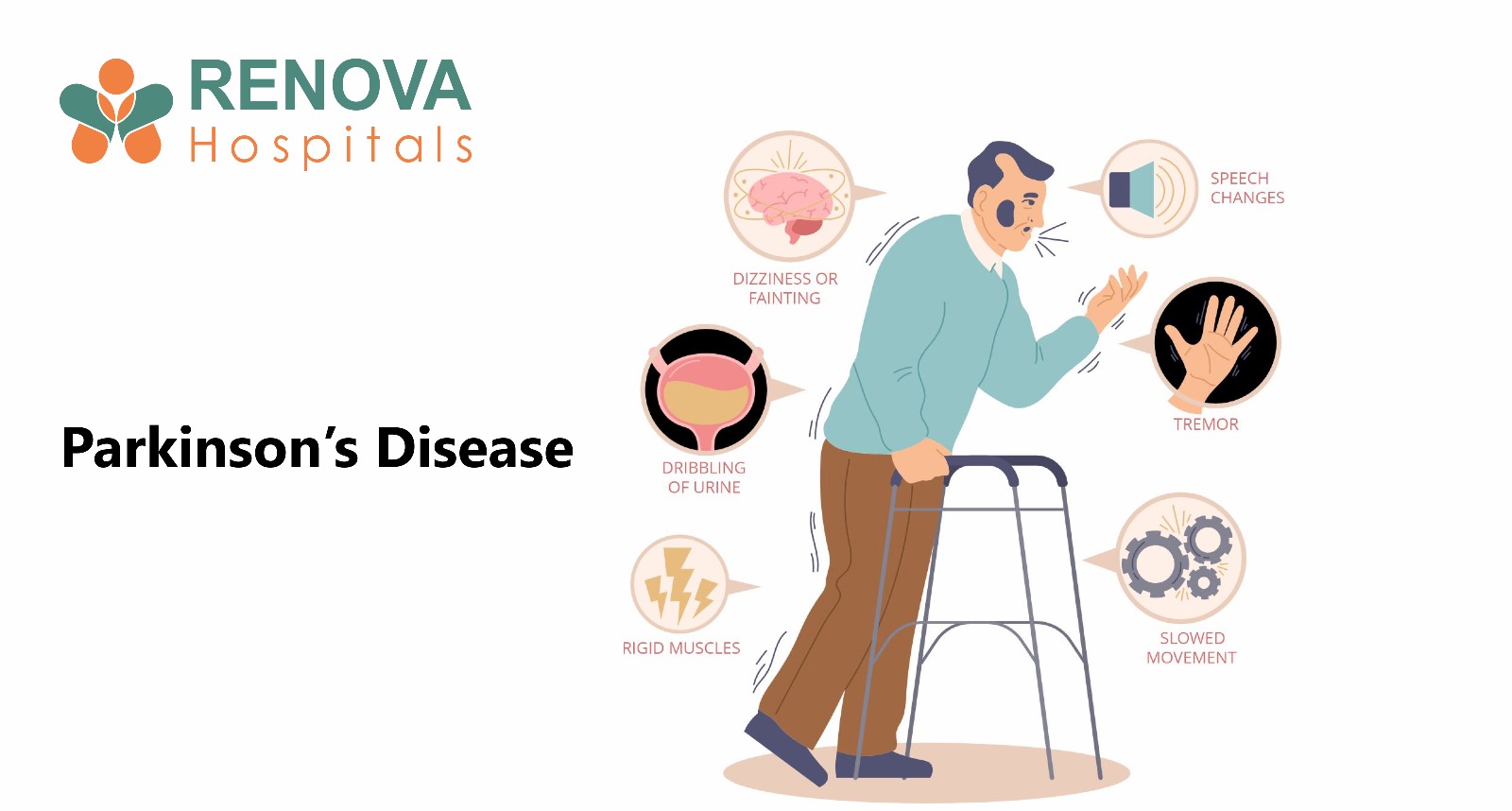
What Are the Early Symptoms of Parkinson’s Disease?
- Resting tremor in one hand
- Slowness of movement
- Muscle stiffness
- Reduced facial expression (masked face)
- Soft or low voice
- Small handwriting (micrographia)
- Loss of smell
- Constipation
- REM sleep behaviour disorder
- Mood changes such as depression or anxiety
Main Motor Symptoms of Parkinson’s Disease
1. Tremor at Rest
Rhythmic shaking, commonly beginning in the hands (pill-rolling tremor).
A persistent, uncomfortable stiffness in your muscles that doesn't seem to go away.
Slowed movement affecting walking, dressing, and daily tasks.
Balance issues increase the risk of falls.
- Shuffling gait (Parkinsonian gait)
- Stooped posture
- Reduced arm swing
- Freezing episodes while walking
Non-Motor Symptoms of Parkinson’s Disease
Common non-motor symptoms include:
- Depression and anxiety
- Cognitive decline or Parkinson’s disease dementia (later stages)
- Sleep disorders
- Constipation and urinary urgency
- Orthostatic hypotension
- Fatigue
- Sexual dysfunction
- Difficulty swallowing
- Chronic pain
What Causes Parkinson’s Disease?
- Dopamine-producing neuron loss
- Alpha-synuclein protein buildup (Lewy bodies)
- Genetic mutations (SNCA, LRRK2, PINK1, PRKN)
- Environmental toxin exposure (pesticides, heavy metals)
- Oxidative stress and mitochondrial dysfunction
Who Is at Risk?
Risk factors include:
- Age above 60 years
- Male gender
- Family history
- Exposure to pesticides or rural toxins
- Previous head injury
How Is Parkinson’s Disease Diagnosed?
Diagnosis is based on:
- Clinical history
- Neurological examination
- Observation of motor symptoms
- Improvement with levodopa therapy
- MRI brain
- Dopamine transporter scan (DaTscan)
- Blood tests to rule out other causes
Can Parkinson’s Disease Be Prevented?
- Exercise regularly; activities like walking, yoga, cycling, or swimming support brain and muscle health.
- Eat a balanced diet, including fruits, vegetables, whole grains, nuts, and adequate fluids.
- Avoid exposure to toxins, and limit contact with pesticides and other harmful chemicals.
- Protect against head injury: wear helmets and follow fall-prevention measures.
- Managing chronic conditions keeps blood pressure, sugar, and cholesterol under control.
Medications for Parkinson’s Disease
Carbidopa-Levodopa
The most effective treatment. It replenishes dopamine in the brain and improves tremor, rigidity, and slowness.
Stimulate dopamine receptors and are often used in the early stages.
Slow dopamine breakdown.
Prolong the levodopa effect and reduce “off periods.”
Helps control dyskinesia (involuntary movements).
Neurologists carefully adjust medication doses to balance symptom control and side effects.
For selected patients with medication-resistant symptoms, Deep Brain Stimulation may be recommended.
DBS involves implanting electrodes in specific brain regions to regulate abnormal signals.
It can significantly reduce tremors and motor fluctuations, but does not cure the disease.
Dietary Requirements for Parkinson’s Disease Patients
- Fresh fruits and vegetables (rich in antioxidants)
- Whole grains
- Lean proteins
- Healthy fats (nuts, seeds, olive oil)
Patients taking carbidopa-levodopa are often advised to:
- Take medication 30–60 minutes before meals
- Distribute protein intake evenly
- Avoid heavy protein meals around medication time
Recommended:
- High-fibre foods (vegetables, oats, legumes)
- Adequate water intake (2–2.5 litres daily unless medically restricted)
- Vitamin D and calcium for bone health
- B-complex vitamins for nerve function
- Soft-textured foods
- Thickened liquids (if recommended)
- Smaller, frequent meals
Rehabilitation & Supportive Care
- Physiotherapy for balance and strength
- Occupational therapy for daily activities
- Speech therapy for voice and swallowing
- Psychological support
- Regular aerobic exercise
When Should You See a Neurologist?
Consult a specialist if you experience:
- Persistent resting tremor
- Slowed movements
- Frequent falls
- Difficulty swallowing
- Loss of smell
- Ongoing sleep disturbances
Parkinson’s Disease Care in Hyderabad – Renova Hospitals
- Experienced neurologists
- Advanced diagnostic imaging
- Personalised medication management
- Deep Brain Stimulation evaluation
- Multidisciplinary rehabilitation services
Medical Disclaimer
In case of a medical emergency, please contact your doctor immediately or visit the nearest hospital
Category
- Joint Replacement
- Joint Replacement
- Joint Replacement
- Joint Replacement
- Joint Replacement
- Joint Replacement