Mumps is a contagious viral infection that most people associate with children, but mumps in adults is a growing concern, often causing more severe symptoms and complications than in younger patients. Since the U.S. mumps vaccination program began in 1967, cases have dropped by more than 99%, yet outbreaks continue to occur, particularly on college campuses, in workplaces, and in close-knit communities.
Whether you are asking "Is mumps contagious?", wondering "How long does mumps last?", or looking for guidance on mumps prevention, this comprehensive guide covers everything you need to know.
Key Takeaways
- Mumps in adults is more serious than in children, with higher risks of orchitis, oophoritis, meningitis, and hearing loss.
- The MMR vaccine (two doses) is ~88% effective and has cut U.S. mumps cases by over 99% since 1967.
- No cure exists; treatment is supportive only. Antibiotics do not work on mumps.
- Mumps spreads before symptoms appear, making vaccination and early isolation critical.
- Good hygiene, no shared utensils, regular handwashing, and covering coughs add a second layer of protection.
What Is Mumps?
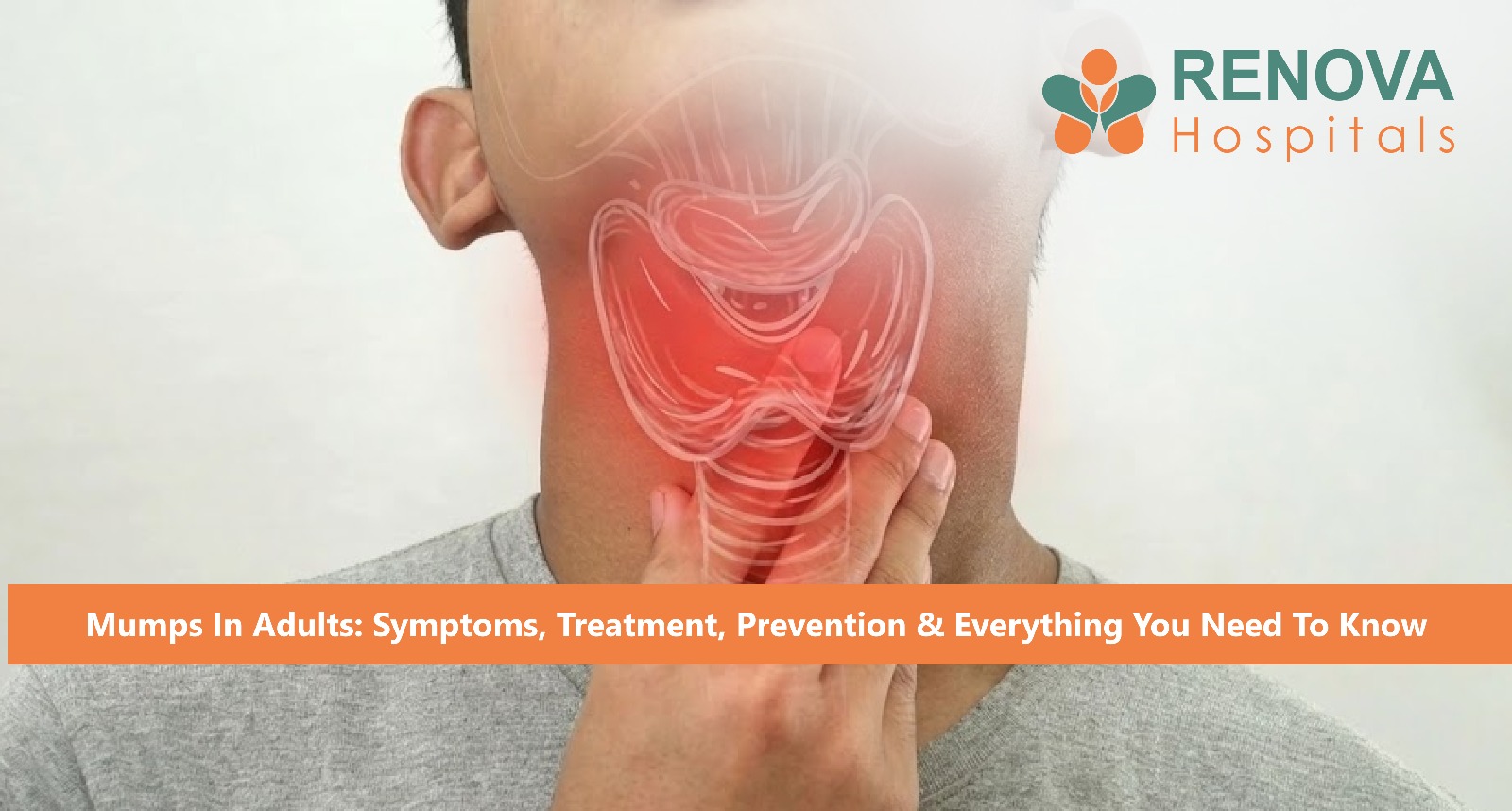
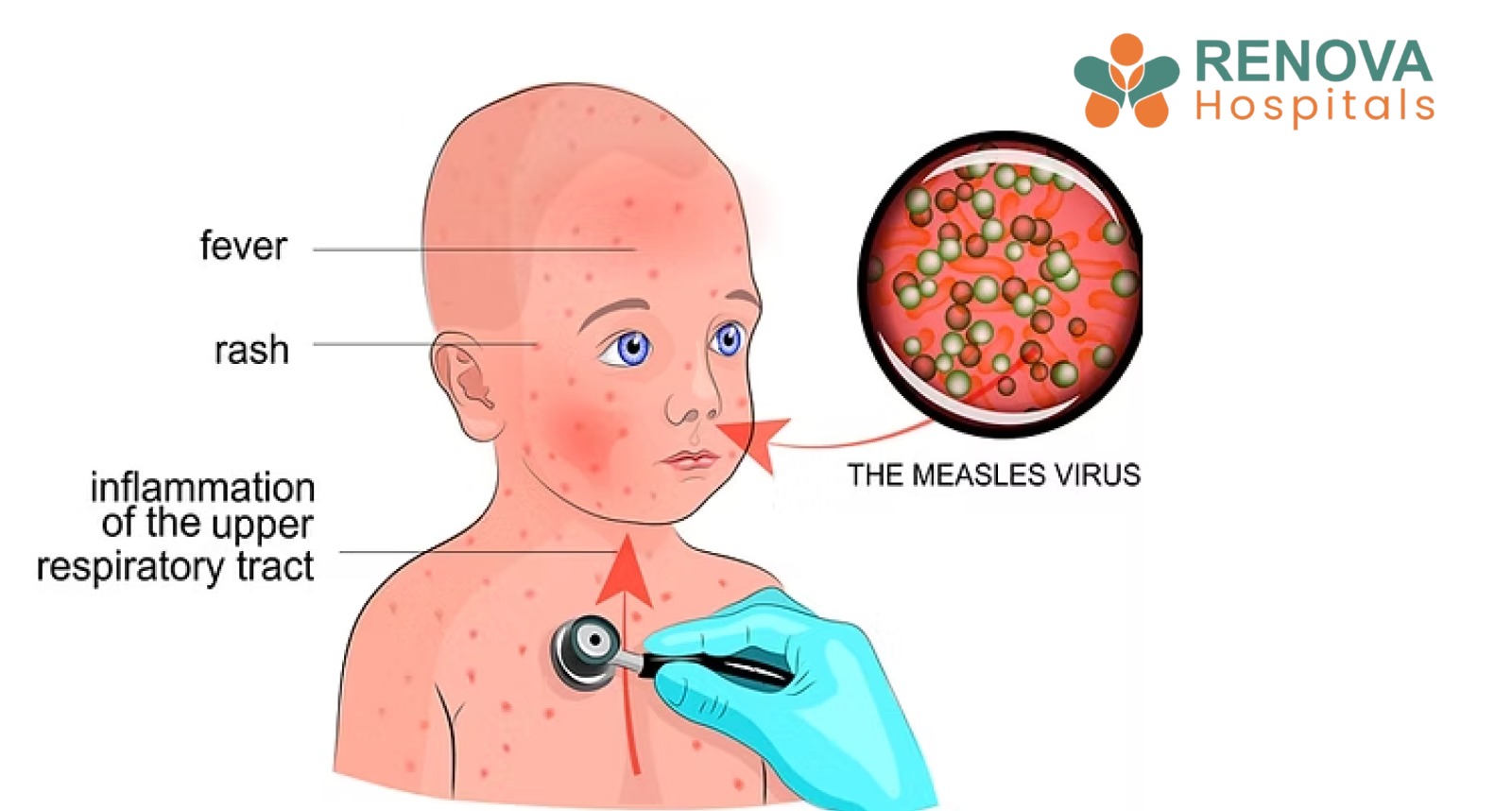
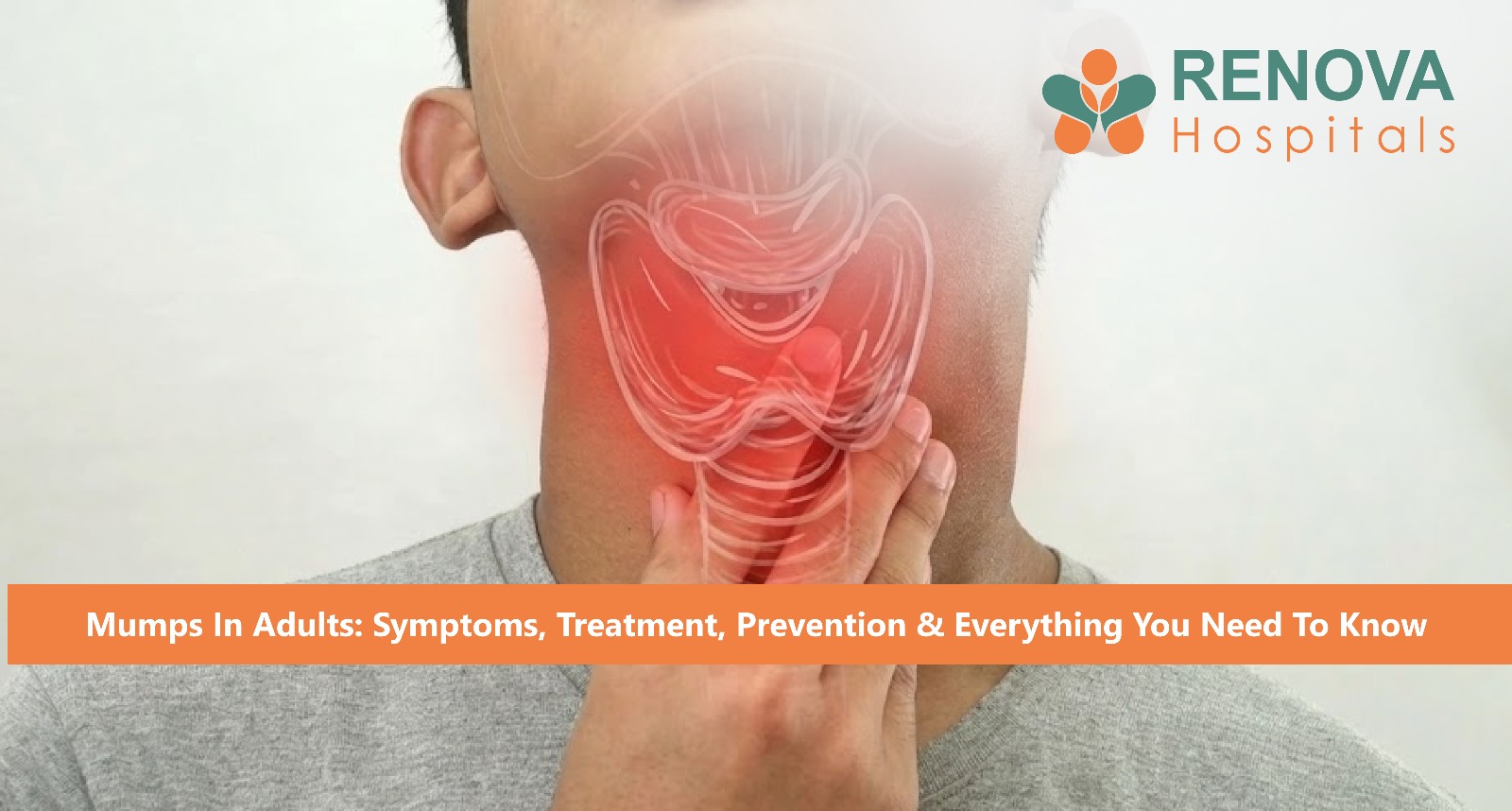
Mumps is caused by the mumps paramyxovirus, which primarily targets the parotid (salivary) glands near the ears, causing painful swelling and the characteristic "chipmunk cheek" appearance. While it can affect anyone, mumps in adults tends to be more serious, with a higher risk of complications compared to young children.
Key Mumps Statistics
• 99%+ decrease in U.S. mumps cases since the 1967 vaccination program (
CDC)
• 152,209 cases were reported in 1968 vs. just 231 in 2003 — a testament to the power of vaccination (
CDC Mumps Outbreaks)
• 34 mumps cases reported across 11 U.S. jurisdictions as of February 27, 2026 (
CDC 2026 Data)
Is Mumps Contagious?
Yes, mumps is highly contagious. It spreads through respiratory droplets and saliva from an infected person. What makes it particularly tricky is that a person can spread the virus from 2 days before symptoms appear to 5 days after, meaning many people unknowingly transmit it before they know they are sick.
The virus spreads through:
• Coughing, sneezing, or talking in close contact
• Sharing utensils, cups, or water bottles
• Kissing or other close physical contact
• Touching contaminated surfaces, then touching the face
Symptoms of Mumps in Adults
Symptoms typically appear 16 to 18 days after exposure (with a range of 12–25 days). In adults, symptoms can be more pronounced than in children.
Early-Stage Symptoms (First 1–3 Days)
• Fever (often above 38°C / 100.4°F)
• Headache and muscle aches
• Fatigue and loss of appetite
• General feeling of being unwell
Characteristic Mumps Symptoms (Days 3–7)
• Painful swelling of the parotid glands (one or both sides of the jaw)
• Puffy, tender cheeks
• Pain when chewing or swallowing
• Tenderness around the ears
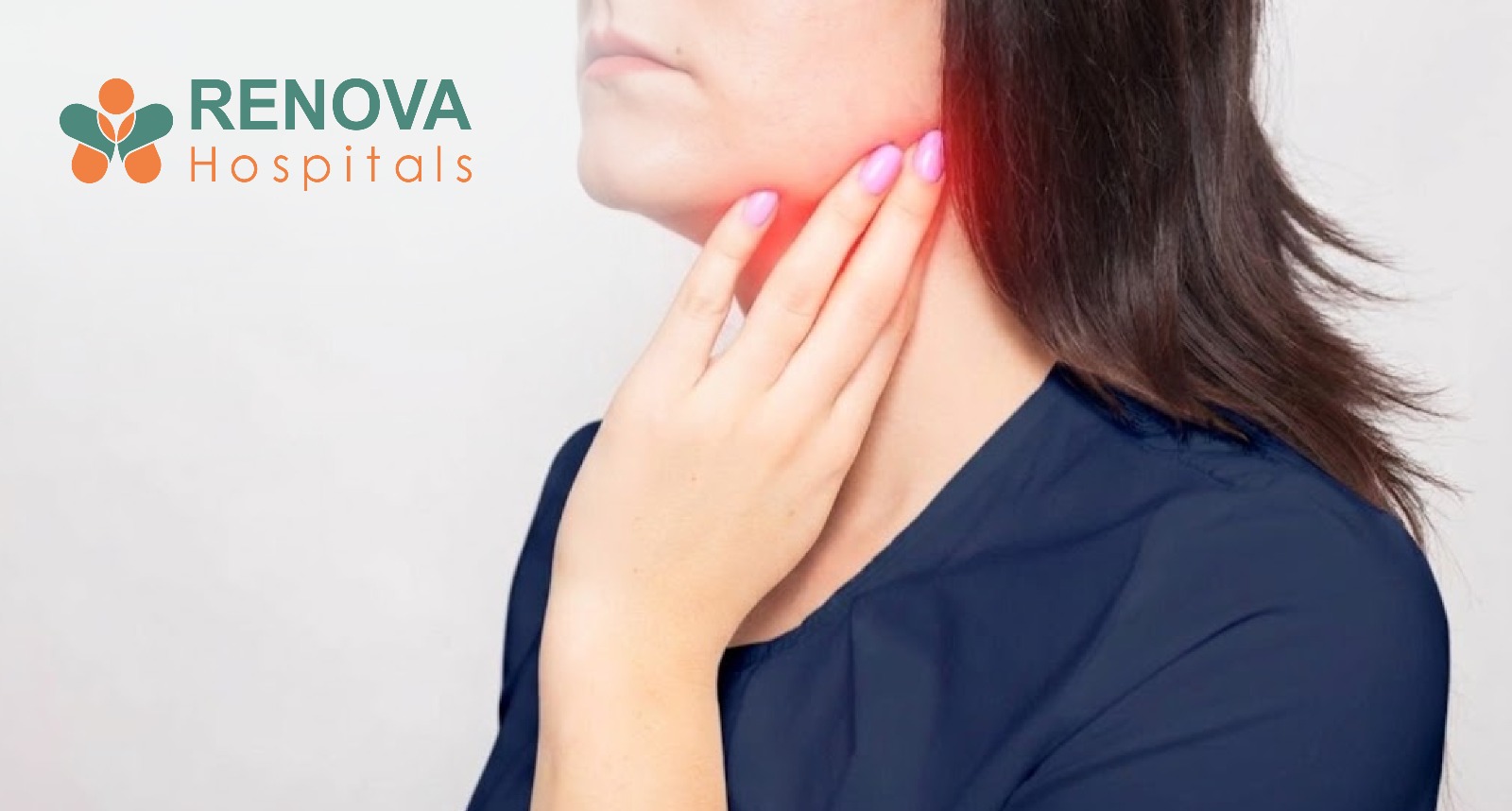
Symptoms of Mumps in Adults - Female-Specific Considerations
Women should be aware that symptoms of mumps in adult female patients can include abdominal pain or pelvic discomfort due to oophoritis (inflammation of the ovaries), which occurs in a small percentage of adult women who contract mumps. While this complication is rare, it should prompt a medical evaluation.
How Long Does Mumps Last?
In most cases, mumps lasts 7 to 10 days. Gland swelling typically improves within one week, and full recovery is usually expected within 2 to 3 weeks. Adults may take longer to recover than children.
How Is Mumps Diagnosed?
Diagnosis is typically based on a physical examination and symptom history. If confirmation is needed, your doctor may order:
• A PCR test (using a saliva or throat swab) — the most reliable laboratory method
• Blood tests to check for mumps antibodies
• Urine tests in some cases
Treatment for Mumps in Adults
There is no specific antiviral drug for mumps. Treatment for mumps in adults focuses on relieving symptoms and supporting recovery:
• Rest and adequate hydration — staying home and keeping fluid intake up is essential
• Pain and fever relief — acetaminophen (paracetamol) or ibuprofen are commonly used
• Warm or cold compresses — applied to swollen glands for comfort
• Soft foods — to reduce pain when chewing
• Salt water gargles — to soothe throat discomfort
Can Antibiotics Treat Mumps?
No. Mumps treatment with antibiotics is not effective because mumps is caused by a virus, not bacteria. Mumps medication is limited to symptom management — there is no antiviral cure. Anyone offering "mumps treatment antibiotics" as a cure is misinformed. If a bacterial secondary infection develops, a doctor may then prescribe antibiotics specifically for that.
Possible Complications — Especially in Adults
Complications are more common in mumps in adults than in young children. Seek medical attention promptly if any of the following occur:
• Orchitis — inflammation of the testicles, occurring in up to 30–40% of post-pubertal males; can rarely affect fertility
• Oophoritis — ovarian inflammation in women; can cause pelvic pain
• Viral meningitis — inflammation of membranes surrounding the brain
• Encephalitis — rare but serious brain inflammation
• Pancreatitis — abdominal pain, nausea, vomiting
• Hearing loss — typically temporary but occasionally permanent
Mumps Prevention: What You Can Do
Get Vaccinated — The Most Effective Strategy
The mumps vaccine is administered as part of the MMR (Measles, Mumps, Rubella) vaccine. According to the
CDC, two doses of the mumps vaccine are approximately 88% effective at preventing mumps, while a single dose offers around 78% protection.
The recommended mumps vaccine schedule:
• First dose: 12–15 months of age
• Second dose: 4–6 years of age
• Adults at high risk (travellers, healthcare workers, college students): should ensure they have received two doses; a third dose may be recommended during outbreaks
Non-Vaccine Prevention of Mumps Disease
Good hygiene plays a crucial role in the prevention of mumps disease, particularly during outbreaks:
• Avoid sharing cups, utensils, or personal items
• Cover coughs and sneezes with a tissue or elbow
• Wash hands regularly with soap and water
• Stay home if you are infected, isolate for at least 5 days after swelling begins
• Ensure your vaccination status is current
When Should You See a Doctor?
Seek medical attention promptly if you or someone you know develops:
• Fever above 39°C (102°F) that does not improve
• Severe or worsening swelling near the jaw or neck
• Difficulty swallowing, speaking, or breathing
• Stiff neck or severe headache
• Testicular or abdominal pain
• Confusion, extreme fatigue, or sensitivity to light
A Note from Renova Hospitals
Mumps is largely preventable, yet it continues to circulate, especially among unvaccinated populations and in crowded settings. If you are unsure of your vaccination status, speak to your doctor about whether you need an MMR dose. Early diagnosis and supportive care can make a significant difference in recovery time and complication rates.
At Renova Hospitals, our infectious disease and pediatric specialists are here to provide expert guidance, rapid diagnosis, and compassionate care. If you notice any symptoms suggestive of mumps, do not wait; consult a healthcare professional promptly.