By Dr. Srinivas Thankari
April 09, 2026
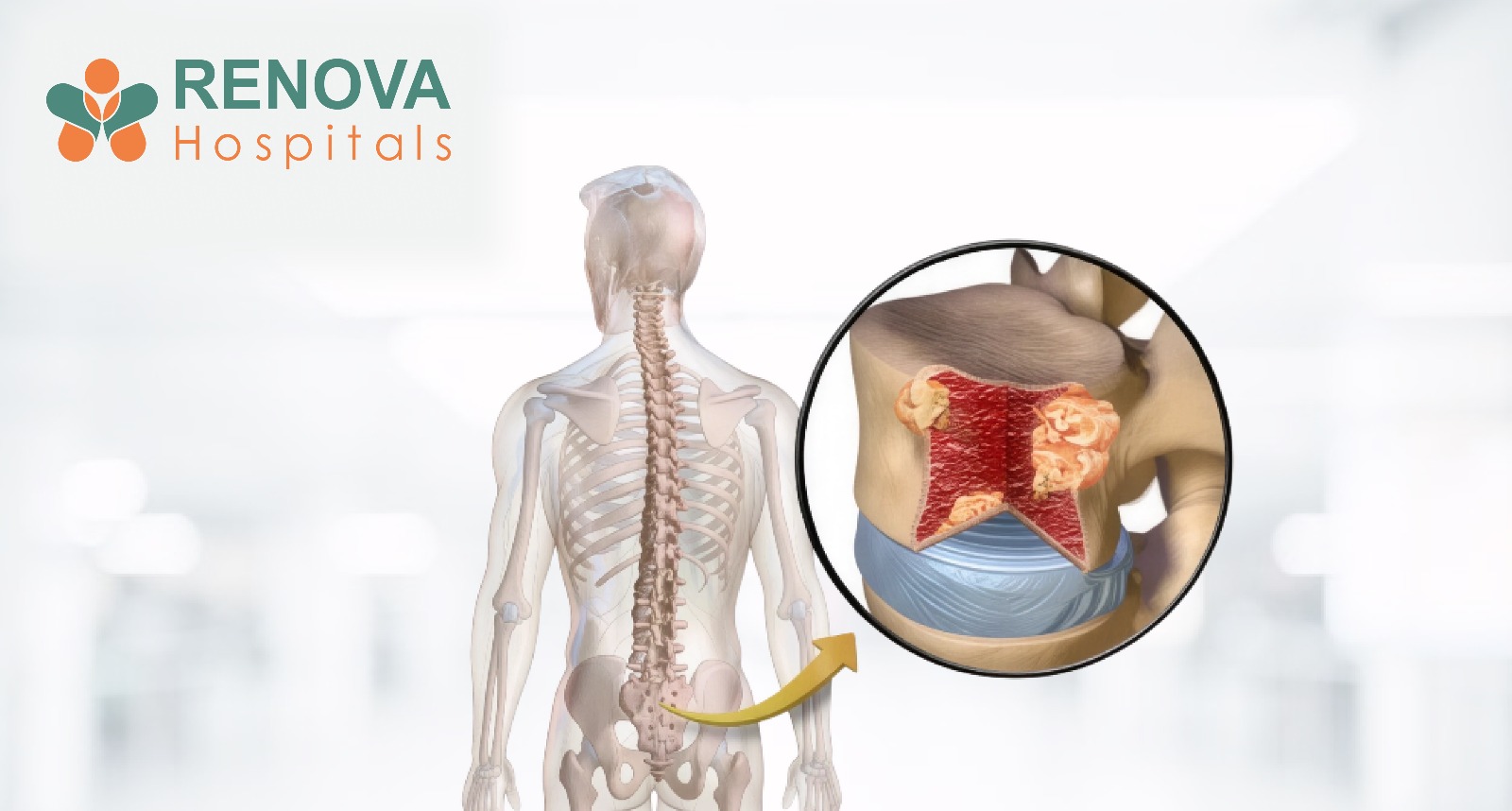
Microdiscectomy: A Minimally Invasive Solution for Herniated Discs
- Microdiscectomy achieves an 86.8% success rate, higher than open discectomy's 77.8%
- Recovery averages 2 weeks, versus 4 weeks with traditional open surgery
- Complication rates are nearly half that of open discectomy (14.9% vs 23%)
- Can be performed as day surgery, with patient satisfaction exceeding 80%
- Reherniation affects 5–21% of patients due to smoking, high BMI, and age
The Growing Problem: Why Herniated Discs Matter
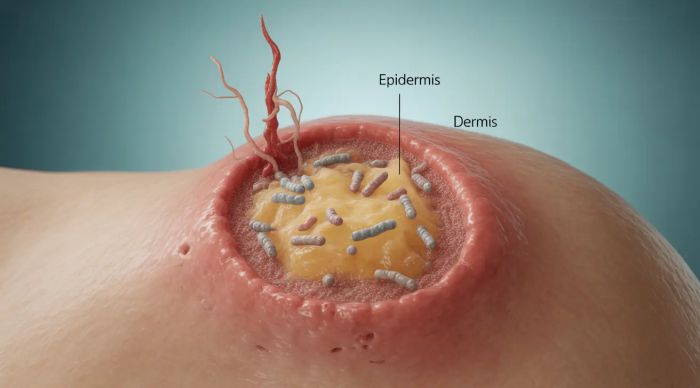
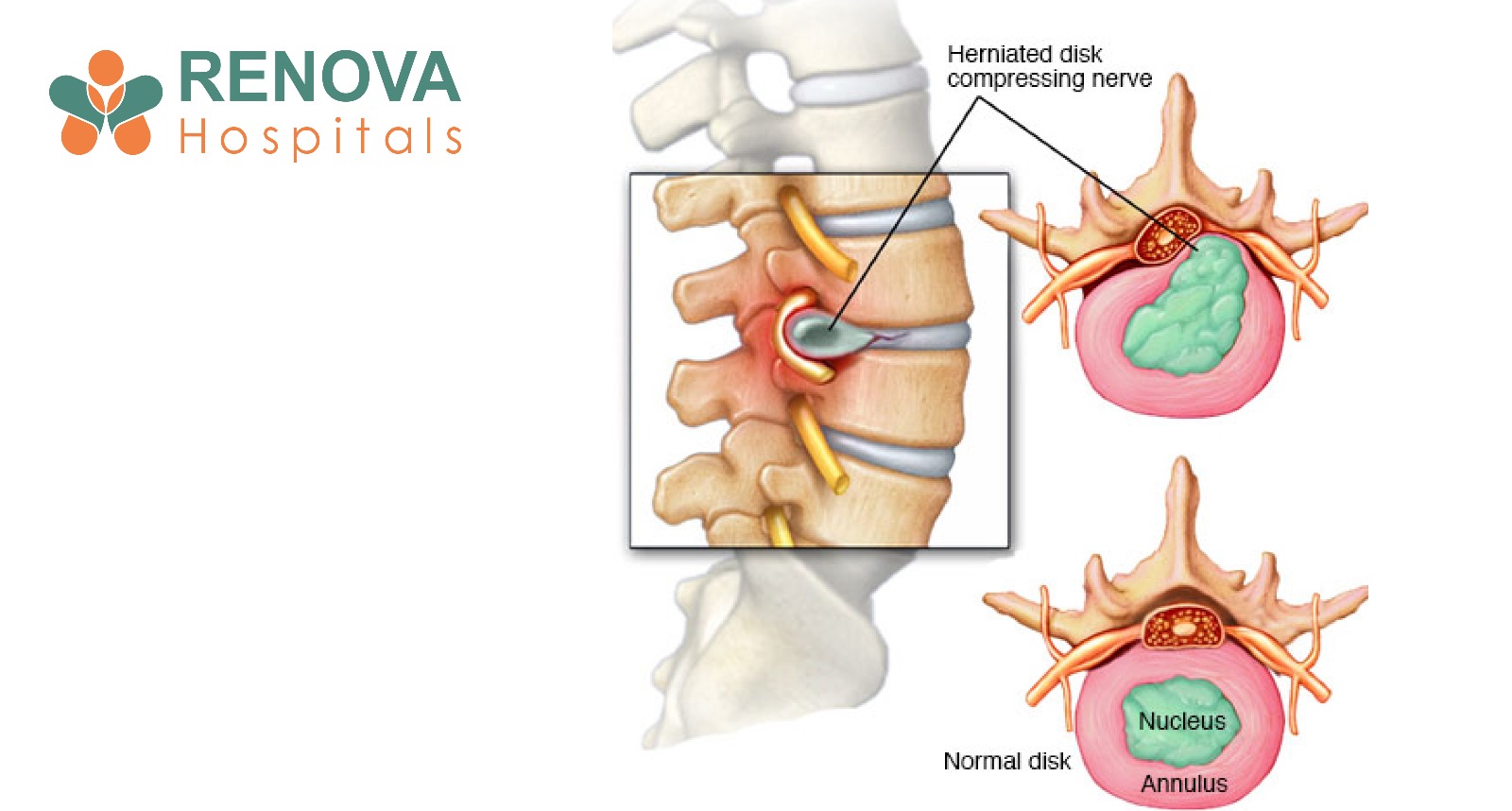
What Is a Herniated Disc?
- Radiating pain down the legs (sciatica) or arms
- Numbness or tingling in the limbs
- Muscle weakness in the affected area
- Loss of bladder or bowel control in severe cases (a surgical emergency)
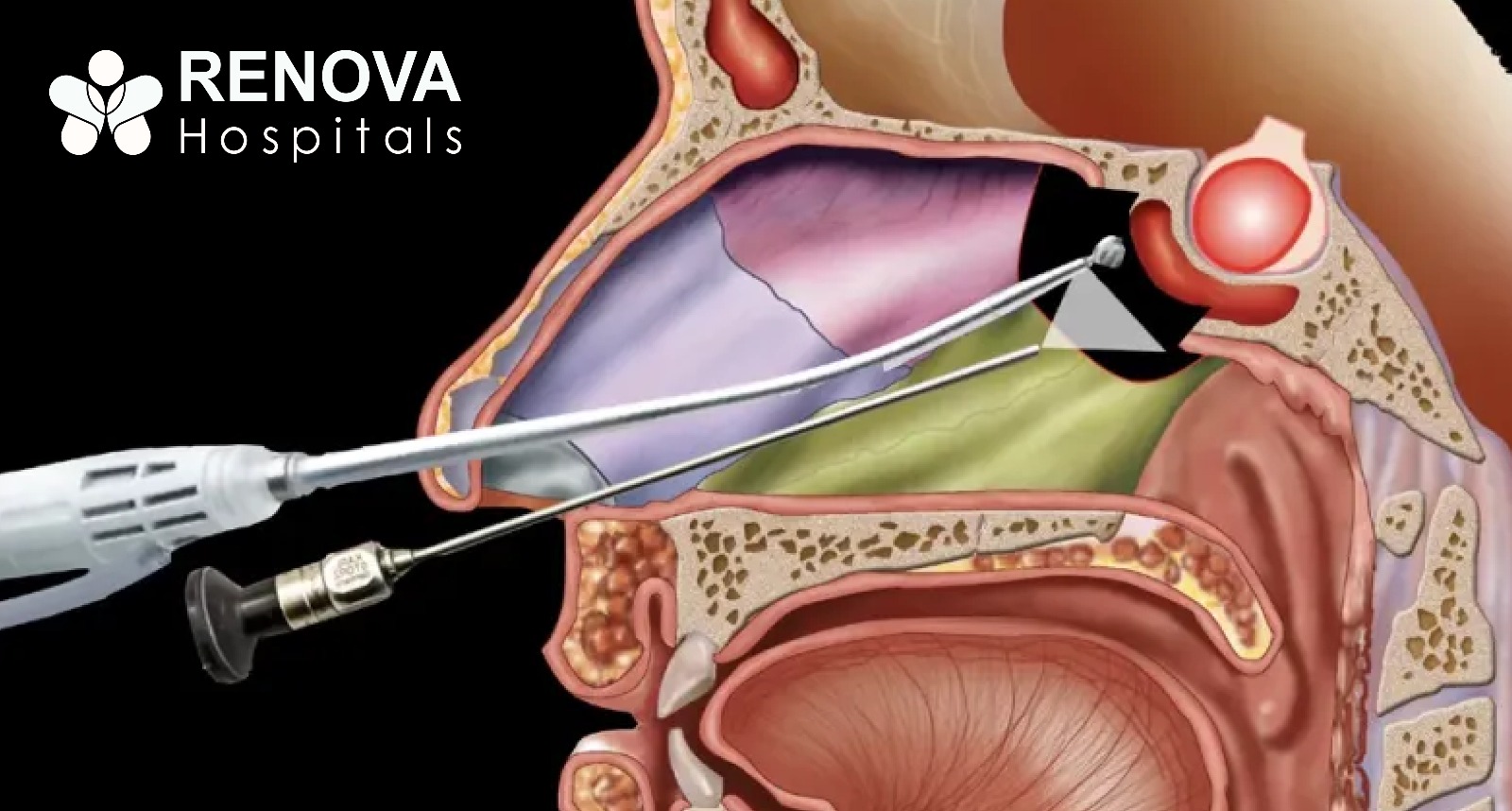
What Is Microdiscectomy Surgery?
- A 1–1.5-inch incision
- A surgical microscope or magnifying loupe for enhanced precision
- Specialised retractors to minimise muscle damage
- General or spinal anaesthesia
Who Is a Candidate for Microdiscectomy?
Progressive Neurological Deficits: Worsening weakness or numbness despite conservative treatment warrants urgent surgical evaluation.
Microdiscectomy Success Rates: What Does the Research Say?
Microdiscectomy vs. Open Discectomy: 2025 Head-to-Head Data
Benefits of Microdiscectomy Over Traditional Surgery
4. Same-Day / Short Hospital Stay Most microdiscectomy procedures can be performed as outpatient or day-surgery procedures, reducing healthcare costs and exposure to hospital-acquired infections.
Post-Operative Care and Recovery
- Most patients are discharged the same day or within 24 hours
- Walking is encouraged from the first day to prevent blood clots and promote circulation
- Pain medication is prescribed as needed; most patients report significant relief of leg pain immediately post-surgery
- Avoid bending, lifting, or twisting the spine
- Light activities (desk work, short walks) can typically be resumed within 1–2 weeks
- Physical therapy usually begins around week 2–3 to strengthen core and spinal muscles
- Driving may be permitted after 2–4 weeks (depending on surgical side and medication)
- Most patients return to sedentary jobs within 2–4 weeks
- Most patients experience significant pain relief within 4 to 6 weeks and full functional recovery within 3–6 months
- Manual or physically demanding jobs typically require 6–12 weeks before return
- A structured physiotherapy programme significantly improves long-term outcomes
Risks and Considerations
- Recurrent disc herniation: Reherniation occurs in approximately 5–21% of patients and is the leading cause of revision surgery. Risk factors include younger age, male sex, high BMI, smoking, and contained disc herniation type.
- Dural tear: An accidental nick in the dura (the membrane surrounding the spinal cord) occurs in a small percentage of cases and is usually repaired during surgery.
- Infection: Risk is very low (less than 1% for discitis with microdiscectomy).
- Nerve damage: Rare due to the magnified visualisation; risk is lower than with open surgery.
- Incomplete relief: A small proportion of patients may not achieve full pain resolution, particularly those with chronic, long-standing nerve compression or significant back pain predominance.
Don't Let Back Pain Define Your Life
The evidence base is robust and growing: microdiscectomy provides superior pain relief, shorter recovery time, and lower complication rates than open discectomy, and offers patients a reliable, safe, and minimally invasive path back to an active, pain-free life.
This blog has been authored by Dr. Srinivas Thankari, an experienced brain and spine surgeon based in Hyderabad. If you are experiencing back pain, sciatica, or nerve-related symptoms, a consultation with a qualified spine specialist can help determine whether microdiscectomy or another treatment approach is right for you.
Category
- Joint Replacement
- Joint Replacement
- Joint Replacement
- Joint Replacement
- Joint Replacement
- Joint Replacement