By Renova Hospitals
March 02, 2026
Prostate Cancer: Symptoms, Stages, Survival Rate & Treatment in India
Quick Summary
- Prostate cancer is the second most common cancer in men worldwide.
- In 2022, there were 1.47 million new cases and 397,000 deaths globally.
- Cases are projected to reach 2.4 million annually by 2040.
- In the United States (2026 estimate), 333,830 new cases and 36,320 deaths are expected.
- In India, while the overall rate of prostate cancer is lower than in the West, many men are unfortunately diagnosed at advanced stages.
- Five-year survival is ~99% for localised disease, but drops significantly in metastatic cases.
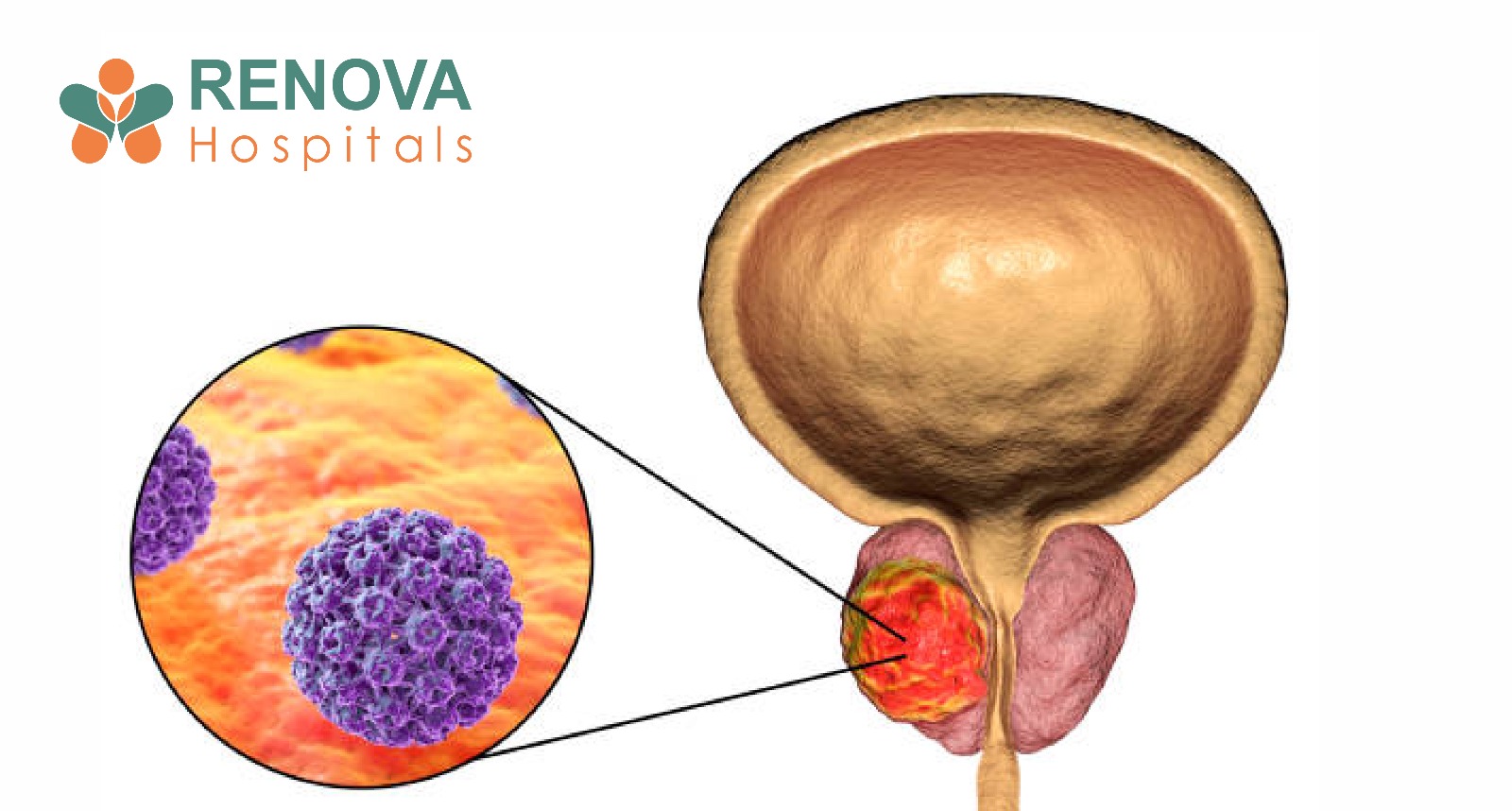
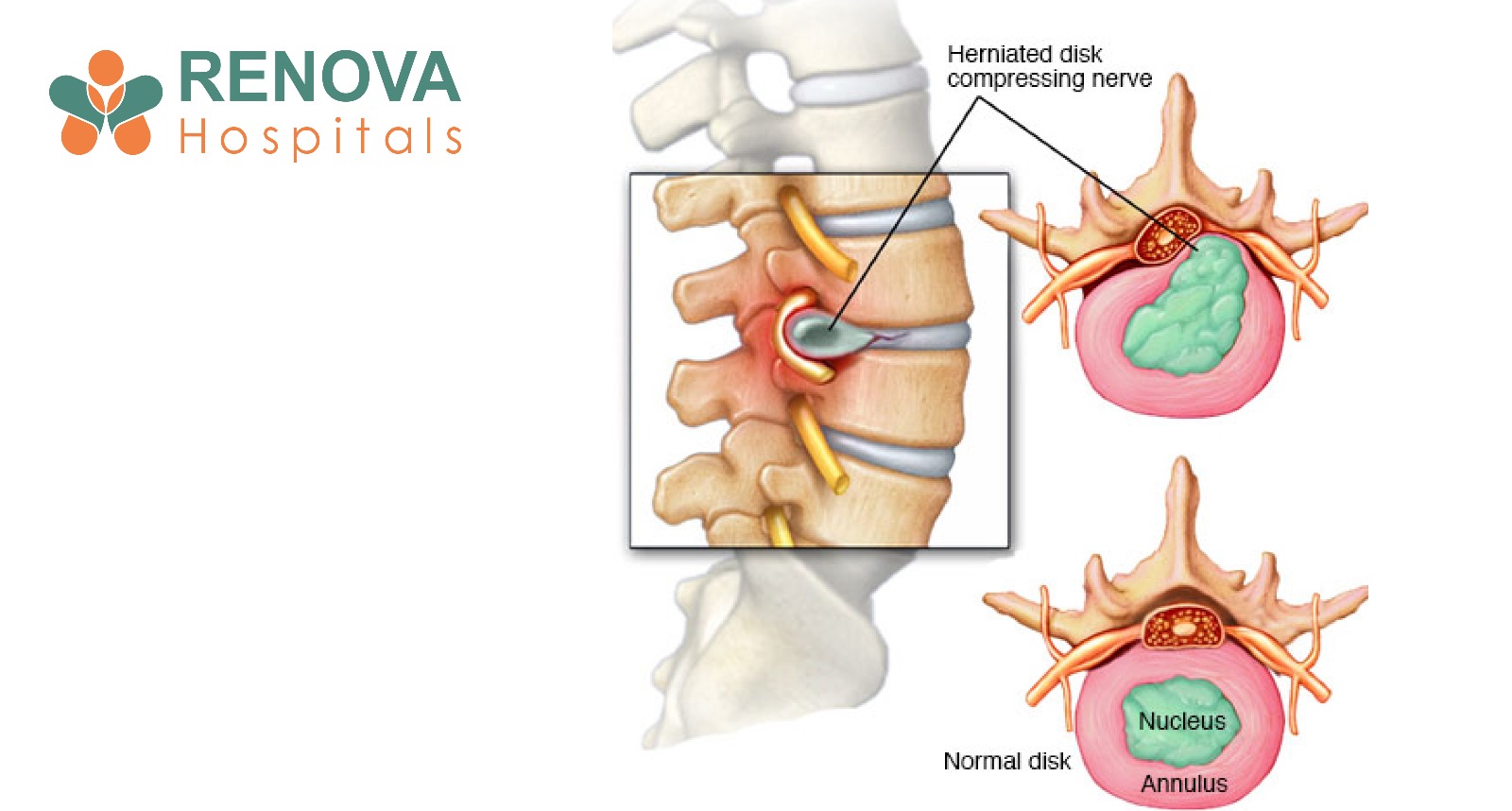
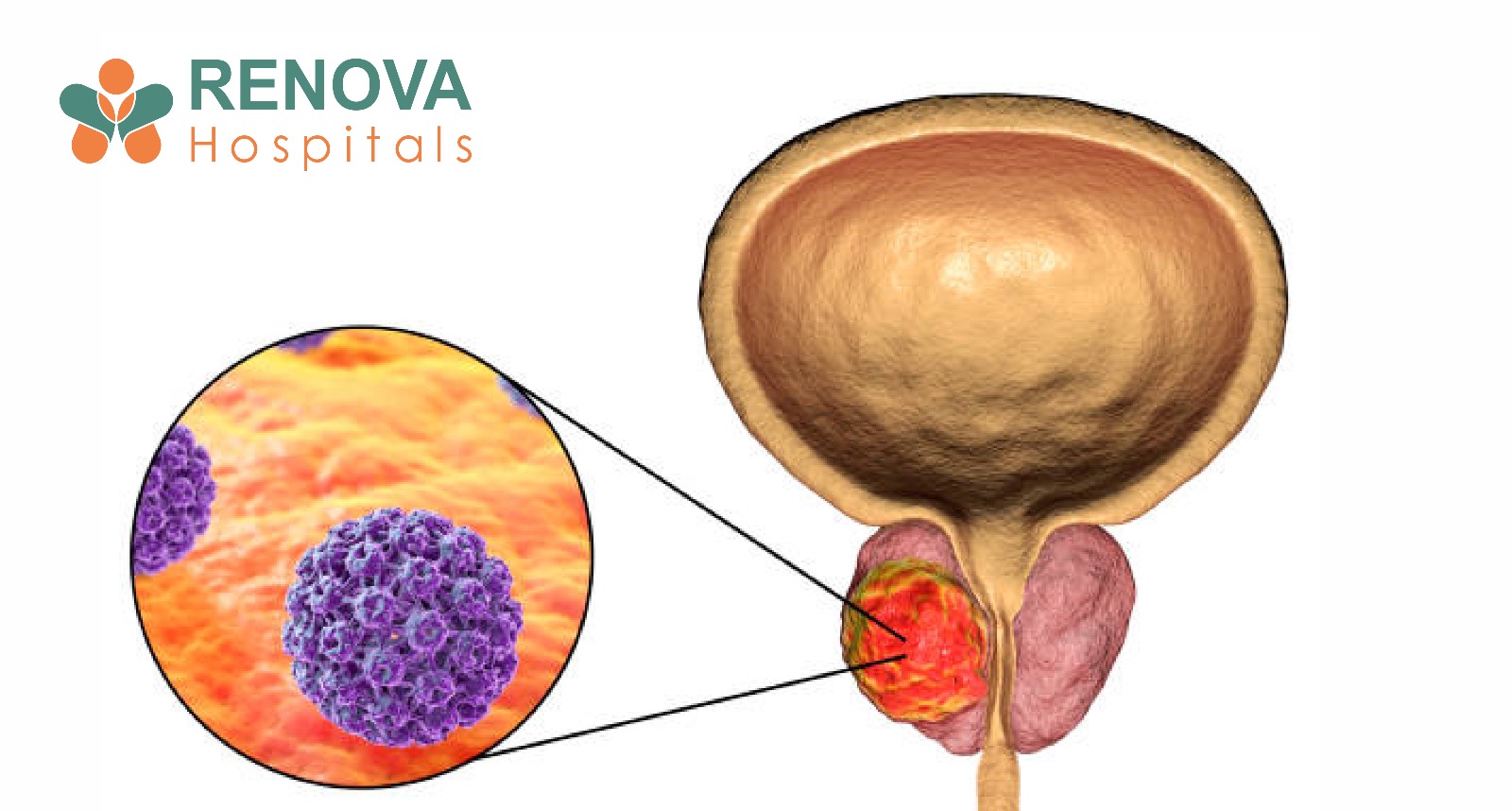
What Is Prostate Cancer?
Prostate cancer develops in the prostate gland, a small walnut-shaped gland below the bladder that produces seminal fluid. Most prostate cancers grow slowly, but some types can be aggressive and spread to bones, lymph nodes, and other organs.
- The 4th most common cancer overall
- The 2nd most common cancer in men
- The 5th leading cause of cancer-related deaths in men
Global & Indian Prostate Cancer Statistics
- 1.47 million new cases in 2022
- 397,000 deaths worldwide
- Projected 2.4 million cases and 712,000 deaths by 2040
- The highest mortality rates are reported in the African region.
- Sadly, men in low-income countries are nearly five times more likely to die from the disease compared to those in wealthier nations.
- 333,830 new cases
- 36,320 deaths
- Lifetime risk: 1 in 8 men
- About 6 in 10 casesare diagnosed after age 65
Why Prostate Cancer is a Growing Concern in India
- Age-standardised incidence rate (ASIR): 5.6 per 100,000
- Mortality rate: 2.7 per 100,000
- There has been a significant rise in overall cases and related deaths since 1990.
- ASIR projected to reach 9.15 per 100,000 by 2031
- The highest incidence was observed in Delhi and Kerala.
- Large regional disparities across Indian states
Risk Factors for Prostate Cancer
- Age (risk rises sharply after 50 years)
- Family history (risk doubles if father affected; triples if brother affected)
- African ancestry / genetic susceptibility
- BRCA1/BRCA2 gene mutations
- ATM, PALB2, CHEK2, mismatch repair genes
- High saturated fat diet
- Obesity
- Sedentary lifestyle
- Possible environmental exposures (cadmium, chemicals)
Symptoms of Prostate Cancer
- Weak or interrupted urine flow
- Frequent urination, especially at night
- Difficulty starting or stopping urination
- Burning or pain during urination
- Blood in urine or semen
- Painful ejaculation
- Persistent lower back, hip, or pelvic pain
- Bone pain (in metastatic disease)
Screening & Diagnosis
- PSA is a blood test used to detect prostate abnormalities.
- USPSTF recommends individual decision-making for men aged 55–69
- Routine screening is not recommended for men over 70
- Declines in PSA screening have been linked to increased advanced-stage diagnoses.
- Multiparametric MRI (mpMRI)
- Transrectal ultrasound (TRUS)-guided biopsy
- MRI fusion biopsy for precise targeting
Staging of Prostate Cancer
- TNM system (Tumour, Node, Metastasis)
- PSA level
- Gleason score tumour aggressiveness grading)
- Localised (Stage I–III): ~99% 5-year survival
- Distant/Metastatic (Stage IV): 34–43% 5-year survival
- Localised: 89% survival
- Locally advanced: 79%
- Metastatic: 41%
- Overall 5-year survival: 61%
- Stage at diagnosis
- PSA level
- Gleason grade
- Treatment completion
Treatment Options for Prostate Cancer
- Regular PSA monitoring
- Periodic imaging
- Avoids overtreatment
- Removal of the prostate gland.
- Best for localised disease.
- External Beam Radiation Therapy (EBRT)
- Often combined with hormone therapy.
- Reduces testosterone levels.
- Common in advanced disease.
- Abiraterone (STAMPEDE trial: 86% alive at 6 years vs 77%)
- Pluvicto (earlier use in trials)
- Pasritamig (under Phase 3 evaluation)
- ANDROMEDA trial combining radiation + targeted therapies
Side Effects of Prostate Cancer Treatment
- Urinary incontinence
- Erectile dysfunction
- Pelvic floor (Kegel) exercises
- Medications for erectile function
- Urinary irritation
- Diarrhoea or rectal discomfort
- Diet changes
- Medications
- Hyaluronic acid rectal spacers to protect the rectum
- Fatigue
- Hot flashes
- Anemia
- Regular exercise
- Medications such as venlafaxine
- Lower risk of incontinence and erectile dysfunction
- Rare complications may occur.
Survival & Prognosis
- Localised disease: Nearly 100% survival
- Regional disease: Excellent outcomes with treatment
- Metastatic disease: 36–43% 5-year survival
- Overall survival in India (hospital-based data): ~61%
Prevention & Risk Reduction
- Low-fat diet
- Increased fruits and vegetables (broccoli, tomatoes)
- Reduced red and processed meat
- Regular exercise (30 minutes daily)
- Maintaining a healthy weight
New technologies are even helping doctors create highly personalised prevention plans based on a patient's unique risk profile.
When Should You See a Doctor?
- Persistent urinary difficulties
- Blood in urine or semen
- Unexplained pelvic or back pain
- Family history of prostate cancer
Medical Disclaimer
Category
- Joint Replacement
- Joint Replacement
- Joint Replacement
- Joint Replacement
- Joint Replacement
- Joint Replacement