Psoriasis is a long-term skin condition that affects millions of people worldwide. While genetics and the immune system play key roles in its development, many patients notice that their symptoms worsen at certain times. These episodes are known as psoriasis flare-ups, and they are often triggered by environmental, lifestyle, or health-related factors.
Understanding your triggers is one of the best ways to manage psoriasis symptoms and prevent frequent flare-ups. By identifying and managing these triggers, patients can reduce inflammation, protect their skin barrier, and maintain better long-term skin health. In this article, we explain the common triggers of psoriasis, why flare-ups occur, and practical strategies to prevent them.
Key Takeaways
- Stress, infections, skin injuries, and lifestyle factors often trigger psoriasis flare-ups
- Triggers are different for everyone, so identifying your personal triggers is important.
- Smoking, alcohol, and a poor diet can worsen symptoms.
- Simple habits like moisturising, managing stress, and maintaining a healthy lifestyle help reduce flare-ups.
- Regular consultation with a doctor helps in better control and long-term management.
What is Psoriasis?
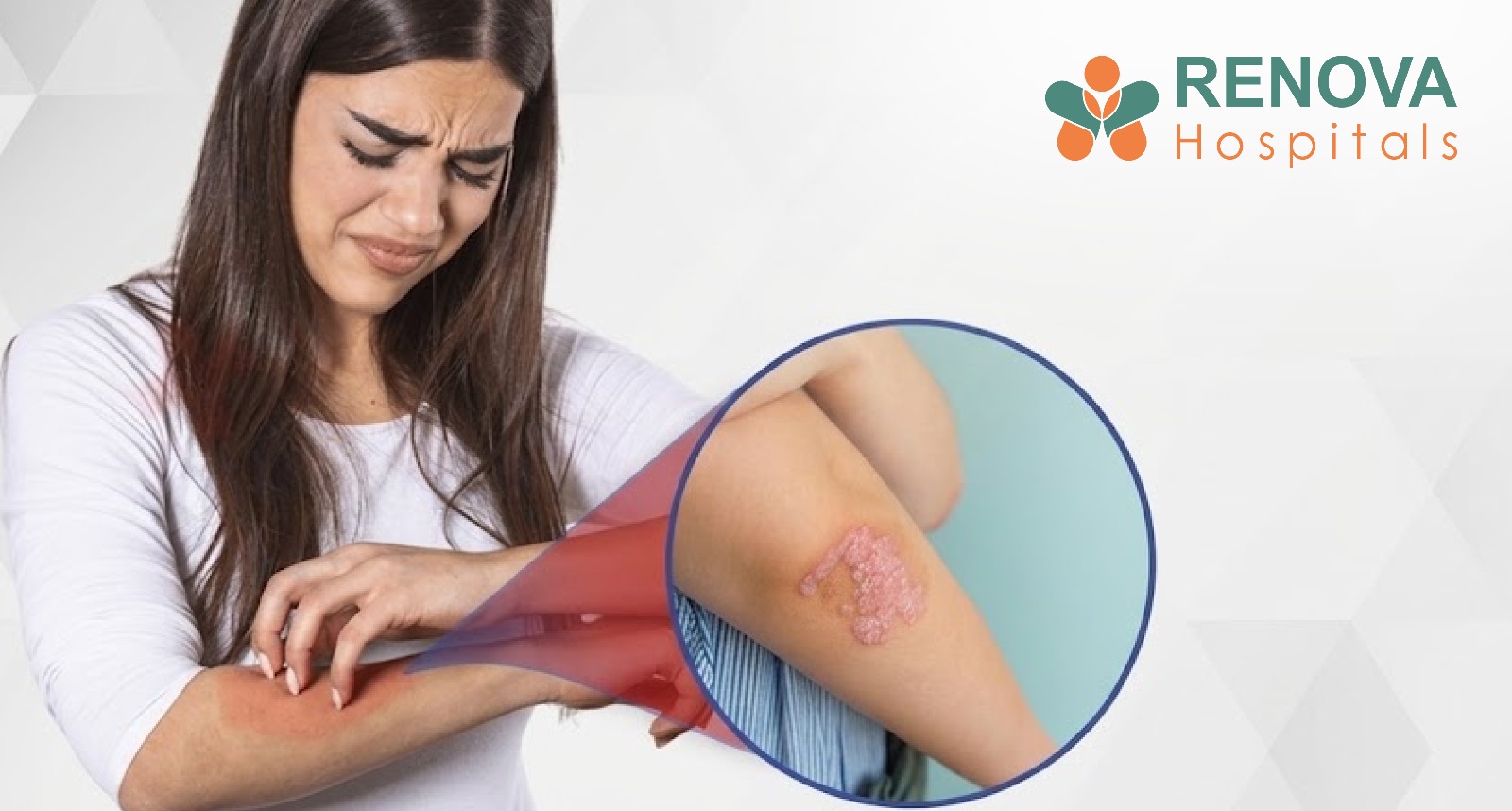
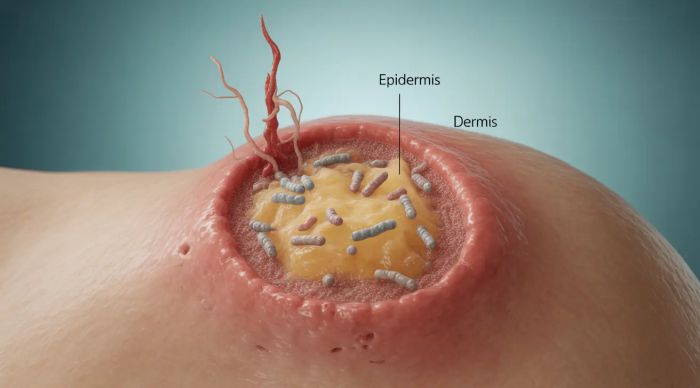
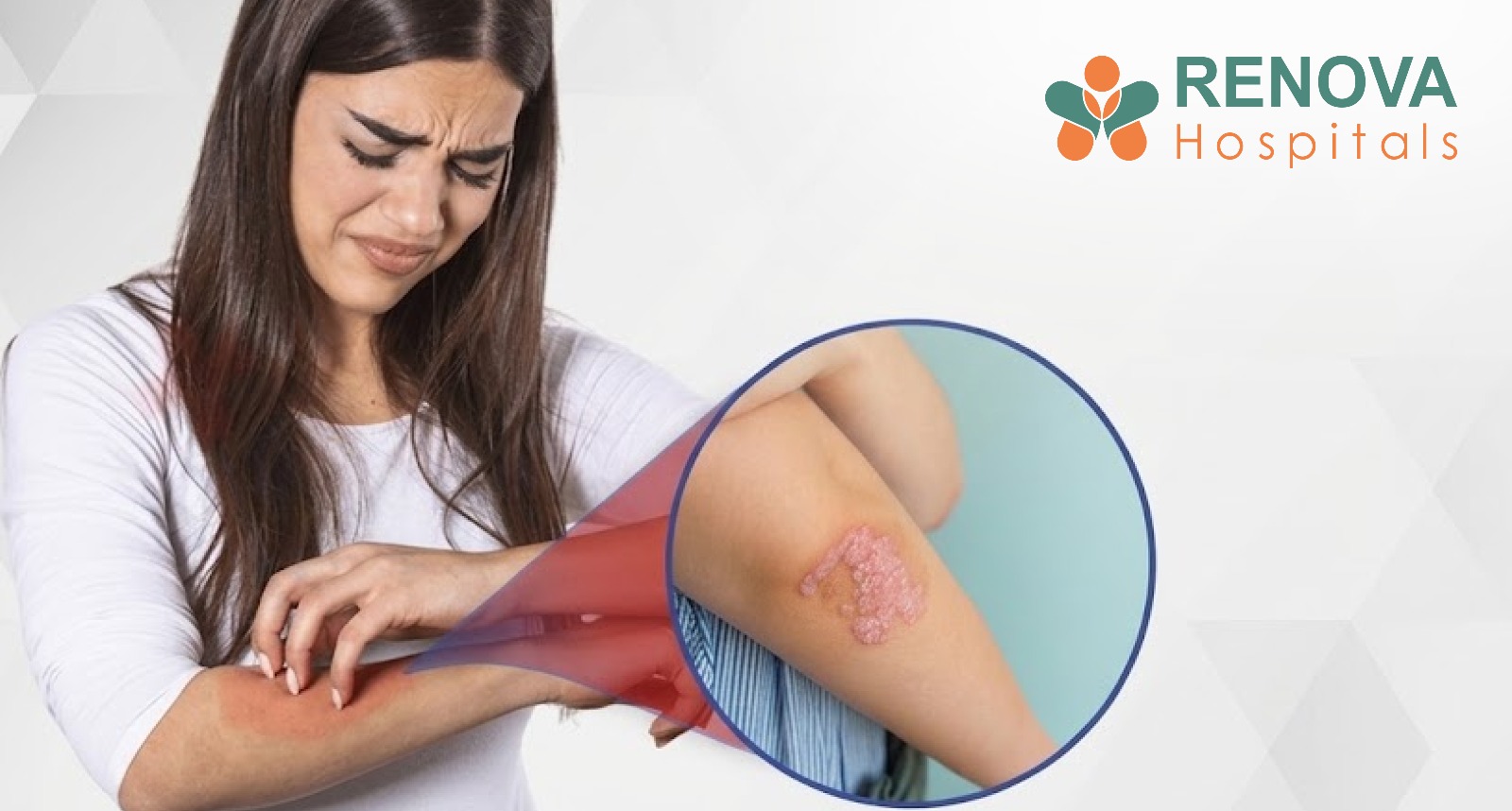
Psoriasis is a chronic autoimmune skin disease in which the immune system mistakenly attacks healthy skin cells. This speeds up the production of new skin cells, which then build up as thick, scaly patches on the skin. These patches often appear on the elbows, knees, scalp, lower back, and nails, and they may cause itching, redness, and discomfort.
Key facts about psoriasis:
- It affects around 2–3% of the global population.
- It is not contagious, meaning it cannot spread through touch or contact.
- Symptoms usually occur in cycles of flare-ups and remission.
- Genetics and immune dysfunction increase susceptibility.
Although psoriasis has no permanent cure, modern dermatology treatments and lifestyle modifications can effectively manage symptoms and reduce flare-ups.
How Psoriasis Develops
Psoriasis usually develops due to a combination of genetic, immune, and environmental factors.
In healthy individuals, skin cells typically renew every 28–30 days. In psoriasis, immune system overactivity causes skin cells to regenerate in
just 3–5 days.
This faster cycle causes skin cells to build up on the surface, forming red, inflamed plaques with silvery scales. Certain triggers can activate this immune response, leading to sudden flare-ups.
Common Psoriasis Triggers
Triggers vary from person to person. Some individuals may experience flare-ups due to stress, while others may notice symptoms after infections, medications, or weather changes.
The most common psoriasis triggers include the following.
1. Stress
Stress is one of the most common triggers of psoriasis flare-ups. When you're stressed, your body releases hormones like cortisol and inflammatory mediators. These chemicals activate immune pathways that increase skin inflammation.
Stress can also worsen itching and discomfort, creating a cycle where stress worsens symptoms and symptoms increase stress.
Common stress triggers include:
- Work pressure
- Emotional trauma
- Lack of sleep
- Anxiety and depression
Stress management techniques such as meditation, breathing exercises, and yoga can help reduce flare-ups.
2. Skin Injury (Koebner Phenomenon)
Skin injuries can trigger psoriasis in the affected area, a reaction known as the
Koebner phenomenon.
Common skin injuries that may cause flare-ups include:
- Cuts or scratches
- Sunburn
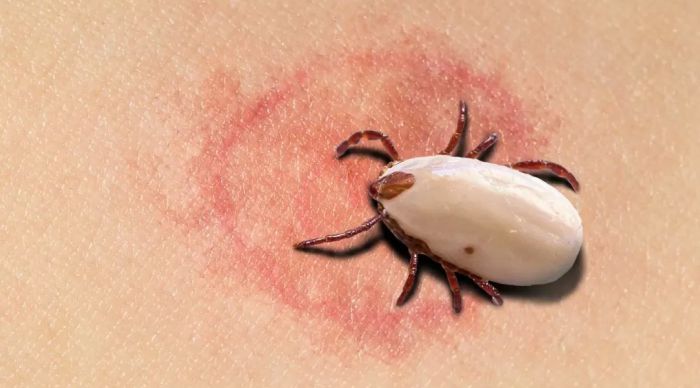
- Insect bites
- Burns
- Tattoos or piercings
- Surgical wounds
Symptoms typically appear 10–14 days after the injury. Protecting the skin from trauma is therefore essential for individuals with psoriasis.
3. Infections
Certain infections can activate the immune system, triggering psoriasis. One of the most common triggers is a streptococcal (strep throat) infection, which can cause a type called guttate psoriasis, particularly in children and young adults.
Other infections associated with psoriasis flare-ups include:
- Strep throat
- Ear infections
- Bronchitis
- HIV infection
- Viral infections such as COVID-19
Infections stimulate immune cells called T-cells, which play a central role in psoriasis inflammation. Prompt treatment of infections may help reduce the risk of flare-ups.
4. Certain Medications
Some
medications can trigger psoriasis or worsen existing symptoms. These drugs may alter immune responses and increase inflammatory pathways in the skin. Patients with psoriasis should always consult their doctor before starting new medications.
5. Cold and Dry Weather
Weather changes can strongly affect psoriasis symptoms.
Cold weather often causes flare-ups because:
- Low humidity dries out the skin
- Indoor heating reduces moisture levels
- Skin barrier damage increases inflammation
Therefore, the winter months tend to worsen psoriasis symptoms in many patients. Keeping the skin moisturised and maintaining indoor humidity can help reduce flare-ups.
6. Smoking
Smoking is strongly associated with both the development and severity of psoriasis.
Research shows that smoking may:
- Increase inflammatory cytokines such as TNF-α and IL-17
- Disrupt immune system regulation
- Worsen skin inflammation
Some studies suggest that smokers may have nearly double the risk of developing psoriasis compared with non-smokers. Quitting smoking can significantly improve skin health and treatment outcomes.
7. Alcohol Consumption
Excessive alcohol intake can also worsen psoriasis.
Alcohol may:
- Increase skin inflammation
- Reduce the effectiveness of psoriasis treatments
- Interfere with medications such as methotrexate
Heavy drinking is therefore considered a major lifestyle trigger for psoriasis flare-ups. Reducing alcohol intake can improve treatment response and disease control.
8. Diet and Metabolic Factors
What you eat can influence psoriasis by affecting your body's inflammation. High intake of processed foods, sugar, and saturated fats may increase inflammatory pathways in the body.
Obesity is another important factor. Fat tissue releases inflammatory molecules called adipokines, which can worsen psoriasis.
Anti-inflammatory diets rich in:
- Fruits and vegetables
- Whole grains
- Omega-3 fatty acids
- Healthy fats
may help reduce flare-ups.
9. Hormonal Changes
Hormonal fluctuations may influence psoriasis symptoms in some individuals.
Examples include:
- Puberty
- Pregnancy
- Menopause
- Low testosterone levels in men
These hormonal shifts can alter immune activity and skin inflammation, sometimes triggering psoriasis symptoms.
Hidden Biological Factors Behind Psoriasis Triggers
Recent research has identified several internal mechanisms that may contribute to psoriasis flare-ups.
Microbiome Imbalance
The skin and gut microbiome play an important role in immune regulation. Changes in microbial diversity can promote inflammatory pathways involving IL-17 and IL-23, which are key drivers of psoriasis.
Immune System Dysregulation
Psoriasis involves overactivation of immune cells called T-helper 17 (Th17) cells. These cells release inflammatory cytokines that cause rapid skin cell growth.
Genetic Susceptibility
Certain genes, including HLA-C*06:02, increase the risk of developing psoriasis. However, genetic risk alone does not guarantee the disease; environmental triggers are usually required to activate it.
How to Prevent Psoriasis Flare-Ups
While it’s not always possible to avoid triggers completely, many lifestyle habits can help reduce flare-ups and improve skin health.
Protect Your Skin
- Use fragrance-free moisturisers daily
- Avoid harsh soaps or irritants
- Take lukewarm showers instead of hot baths
- Apply broad-spectrum sunscreen (SPF 30+) to prevent sunburn
A healthy skin barrier is essential for preventing flare-ups.
Manage Stress Effectively
Stress reduction can significantly improve psoriasis control.
Helpful strategies include:
- Meditation and mindfulness
- Yoga or relaxation exercises
- Support groups or counselling
- Maintaining a healthy work-life balance
Adequate sleep is also important. Adults should aim for 7–9 hours of sleep per night.
Follow an Anti-Inflammatory Diet
A balanced diet may help reduce inflammation.
Recommended foods include:
- Fatty fish (salmon, sardines)
- Flaxseeds and walnuts
- Fresh fruits and vegetables
- Whole grains
- Olive oil
Limiting processed foods, red meat, sugar, and alcohol can help reduce inflammation.
Maintain a Healthy Weight
Weight management plays a major role in psoriasis control.
Regular physical activity:
- Reduces systemic inflammation
- Improves immune regulation
- Supports mental well-being
Experts recommend at least 30 minutes of moderate exercise most days of the week.
Treat Infections Promptly
Because infections can trigger psoriasis flare-ups, early medical treatment is important. If symptoms such as sore throat, fever, or
skin infections appear, consult a healthcare provider promptly.
Work With a Dermatologist
Managing psoriasis effectively requires a personalised treatment plan.
Dermatologists may recommend:
- Topical medications
- Phototherapy
- Oral medications
- Biologic therapies targeting immune pathways such as IL-17 and IL-23
Regular medical follow-up helps ensure optimal disease control.
When to See a Doctor
You should see a doctor if:
- Skin rashes become widespread or painful
- Symptoms interfere with sleep or daily activities
- Psoriasis does not improve with treatment
- Joint pain or swelling occurs (possible psoriatic arthritis)
Early diagnosis and treatment can prevent complications and improve quality of life.
Conclusion
Psoriasis is a complex condition influenced by your genes, immune system, and everyday triggers. While the disease cannot be completely cured, understanding and managing triggers can significantly reduce flare-ups. Common triggers such as stress, infections, skin injuries, medications, smoking, alcohol, and weather changes can all activate the immune system and worsen symptoms.
With the right lifestyle habits, protecting the skin, and working closely with a dermatologist, individuals with psoriasis can effectively control flare-ups and maintain healthier skin. If you experience persistent skin symptoms or frequent flare-ups, consulting a dermatologist can help you receive an accurate diagnosis and a personalised treatment plan
Expert Dermatology Care at Renova Hospitals
At
Renova Hospitals, our
dermatology specialists offer expert care for psoriasis and other chronic skin conditions. We combine advanced diagnostics, personalised treatment plans, and modern therapies designed to help patients manage symptoms effectively and improve their quality of life.
If you are experiencing symptoms of psoriasis or frequent flare-ups, consult our dermatology experts for an accurate diagnosis and an appropriate treatment plan
Medical Disclaimer
This information is intended for general awareness and should not replace professional medical advice. Please consult a qualified healthcare professional for diagnosis and treatment.