By Renova Hospitals
March 10, 2026
Can Fatty Liver Disease Increase Your Risk of Liver Cancer?
Understanding this connection can help with early detection, prevention, and timely treatment.
- Fatty liver disease may increase the risk of liver cancer and some other cancers.
- Long-term liver inflammation and scarring can increase the risk of cancer development.
- NAFLD and AFLD are both linked to hepatocellular carcinoma (HCC).
- Early lifestyle changes can reverse fatty liver disease in many cases.
- Regular screening is important for people with metabolic risk factors.
What Is Fatty Liver Disease?
Fatty liver disease occurs when excess fat builds up in liver cells, which can affect how the liver works over time.
The two main types of fatty liver disease include:
- Obesity
- Type 2 diabetes
- High cholesterol
- Insulin resistance
- Metabolic syndrome
Alcohol-Related Fatty Liver Disease (AFLD)
Can Fatty Liver Lead to Cancer?
Yes. Fatty liver disease can increase the risk of hepatocellular carcinoma (HCC), the most common type of liver cancer.
This stage involves:
- Liver inflammation
- Liver cell damage
- Early fibrosis (scar tissue formation)
Stage 3: Liver Fibrosis
Stage 4: Cirrhosis
How Fatty Liver Increases Liver Cancer Risk
Some biological mechanisms explain the link between fatty liver disease and cancer.
- DNA damage
- Genetic mutations
- Abnormal cell growth
The liver normally filters toxins from the blood. Fat buildup can reduce the liver’s ability to neutralise harmful substances, increasing cancer risk.
How Common Is Liver Cancer in People With Fatty Liver Disease?
Studies suggest that people with fatty liver disease have a significantly higher risk of liver cancer.
- Some studies suggest that people with NAFLD may have a higher risk of hepatocellular carcinoma compared with the general population.
- People with alcohol-related fatty liver disease may have a 2–2.6 times higher risk of liver cancer.
- Early-onset NAFLD (before age 45) is associated with increased risk of multiple cancers.
Globally, liver cancer remains one of the leading causes of cancer deaths, with more than 800,000 new cases each year.
Fatty Liver Disease and Other Types of Cancer
Some studies suggest that fatty liver disease may also be associated with a higher risk of certain cancers.
- Colorectal cancer
- Kidney cancer
- Bladder cancer
- Uterine cancer
- Oral and throat cancers
- Esophageal cancer
- Pancreatic cancer
- Lung cancer
- Thyroid cancer
- Leukemia
Symptoms of Cancer Related to Fatty Liver Disease
Fatty liver disease usually causes no symptoms in its early stages. However, when liver cancer develops, some people may experience symptoms such as:
- Jaundice (yellowing of skin and eyes)
- Loss of appetite
- Unexplained weight loss
- Persistent fatigue
- Flu-like symptoms
- A lump or swelling on the right side of the abdomen
When Should You Seek Medical Help?
You should consult a doctor if you experience:
- A persistent lump in your abdomen
- Unexplained weight loss
- Ongoing fatigue
- Symptoms of liver disease that last more than two weeks
- Severe jaundice
- Continuous vomiting for more than 48 hours
How Doctors Diagnose Liver Cancer
- Liver enlargement
- Abdominal swelling
- Jaundice
- Alpha-fetoprotein (AFP)
- Ultrasound
- CT scan
- MRI scan
Treatment Options for Liver Cancer
Treatment depends on the stage of cancer and the patient’s overall health.
- Surgery to remove tumours
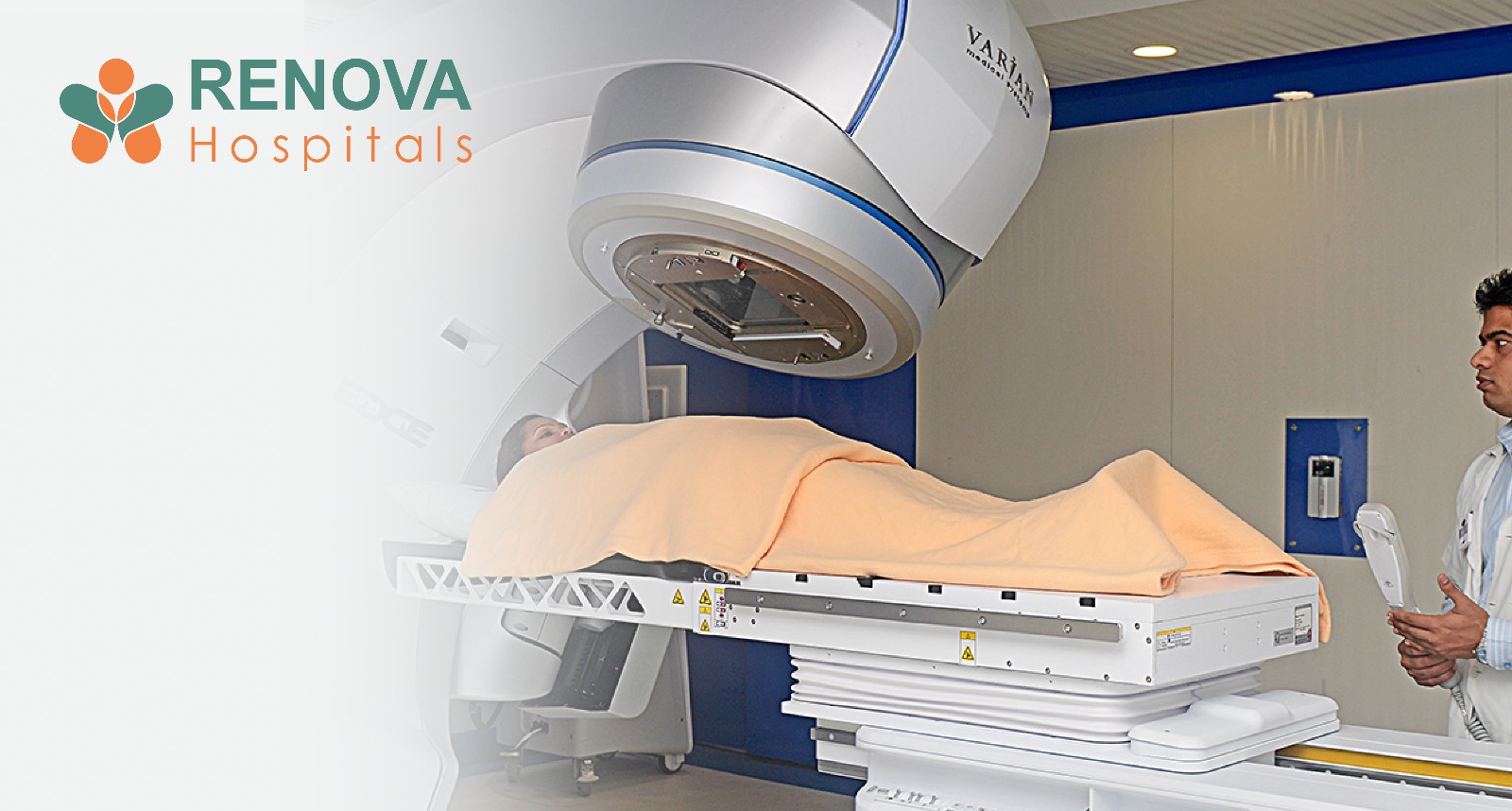
- Radiation therapy
- Targeted drug therapy
- Immunotherapy
- Chemotherapy
- Ablation therapy
- Embolization therapy
Can Fatty Liver Be Misdiagnosed as Cancer?
In some cases, fatty liver deposits may appear similar to tumours on imaging scans, such as ultrasound or CT. This can occasionally lead to diagnostic confusion.
- Additional imaging tests
- Blood tests
- Liver biopsy
These tests help confirm the correct diagnosis.
Can Cancer Be Mistaken for Fatty Liver?
Yes. In some cases, early liver tumours may appear similar to fatty liver disease on imaging. Because of this overlap, doctors often use multiple diagnostic tools to ensure an accurate diagnosis.
Can Fatty Liver Disease Be Prevented From Leading to Cancer?
The good news is that fatty liver disease is often reversible in its early stages.
A healthy diet should include:
- Fruits and vegetables
- Whole grains
- Lean proteins
- Healthy fats
Why Early Screening Is Important
Fatty liver disease is often called a “silent disease” because it rarely causes symptoms until advanced stages.
Regular screening is especially important for people with:
- Obesity
- Type 2 diabetes
- High cholesterol
- Family history of liver disease
Expert Liver Care at Renova Hospitals
At Renova Hospitals, our specialists provide advanced diagnosis and treatment for liver diseases, including:
- Fatty liver screening
- FibroScan and advanced imaging
- Liver cancer detection
- Personalised treatment plans
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional or specialist for diagnosis and treatment.
Category
- Joint Replacement
- Joint Replacement
- Joint Replacement
- Joint Replacement
- Joint Replacement
- Joint Replacement