By Renova
March 27, 2026
Mouth Ulcers: Why Do You Get Them Frequently?
Key Takeaways
- Mouth ulcers (aphthous ulcers/canker sores) are common but become a concern when they recur frequently.
- Key causes include deficiencies in Vitamin B12, iron, and folate, which are correctable with simple blood tests and supplementation.
- Chronic stress, hormonal changes, food triggers, and minor oral injuries are among the most common lifestyle-related causes.
- Recurring ulcers may be a symptom of underlying conditions such as coeliac disease, Crohn's disease, Behçet's disease, or lupus.
- Most ulcers heal within 7–14 days; any that last more than 3 weeks require medical evaluation.
- Switching to an SLS-free toothpaste, managing stress, and eating a nutrient-rich diet are proven prevention strategies.
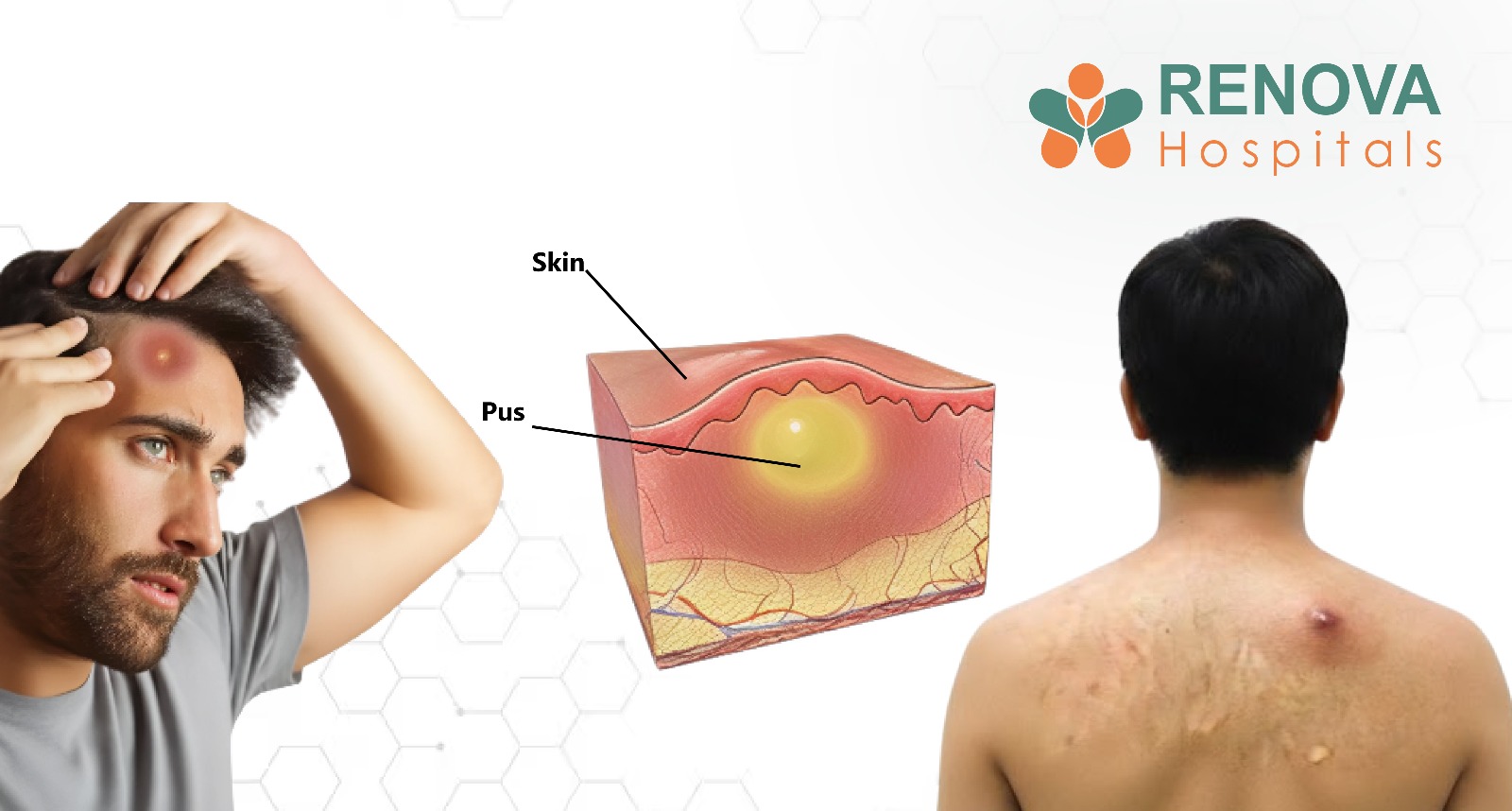
What Are Mouth Ulcers?
Types of Mouth Ulcer
Not all mouth ulcers are the same. Recognising the type can help determine the cause and guide treatment.
These are the most common type, accounting for around 80% of cases. They are small (usually under 10mm), round or oval, and heal without scarring within one to two weeks. While painful, they are typically manageable and do not indicate serious disease.
Major Aphthous Ulcers
Larger and deeper than minor ulcers, these can be extremely painful and take three to six weeks to heal. They may leave behind scar tissue and are associated with conditions such as Crohn's disease or immunosuppression.
Despite their name, these have no relation to the herpes virus. They appear as clusters of multiple tiny ulcers (sometimes 10–100 at once), which may merge to form irregular, larger sores. They are intensely painful and more common in women and older adults.
One of the leading causes of recurrent mouth ulcers is inadequate nutrition, particularly deficiencies in:
- Vitamin B12 is essential for DNA synthesis and the repair of mucosal cells
- Iron is critical for oxygen transport to tissues and immune function
- Folate (Vitamin B9) is vital for cell growth and tissue maintenance
- Zinc supports wound healing and the structural integrity of oral tissues
The relationship between mental health and oral health is well-established. Chronic stress triggers the release of cortisol and other inflammatory mediators that suppress immune function and delay tissue repair. Sleep deprivation compounds this further by reducing the body's overnight healing processes.
The delicate lining of the mouth can be disrupted by everyday incidents, including:
- Accidentally biting your cheek, tongue, or lip
- Aggressive tooth brushing with a hard-bristle brush
- Sharp-edged food like crisps, crackers, or hard toast
- Ill-fitting dentures or orthodontic braces
- Dental procedures such as extractions or injections
Certain foods are well-recognised triggers for mouth ulcers in susceptible individuals:
- Spicy foods, including chillies, hot sauces, and heavily spiced dishes
- Citrus fruits: oranges, lemons, limes, grapefruit
- Acidic foods: tomatoes, vinegar-based condiments, pineapple
- Gluten in individuals with undiagnosed coeliac disease
- Nuts and chocolate are reported triggers in some individuals
Women are statistically more likely to experience recurrent mouth ulcers, suggesting a hormonal component. Ulcers may coincide with specific phases of the menstrual cycle, typically appearing in the luteal phase (the week before menstruation). Pregnancy and perimenopause may also influence ulcer frequency due to fluctuating oestrogen and progesterone levels, which affect immune regulation and mucosal sensitivity.
In some patients, particularly those with frequent, severe, or treatment-resistant ulcers, the recurrence may be a symptom of an underlying systemic condition. These include:
- Coeliac disease is a gluten intolerance that damages the gut lining and depletes nutrients
- Crohn's disease is a chronic inflammatory bowel condition that can affect any part of the gastrointestinal tract, including the mouth
- Ulcerative colitis is another inflammatory bowel disease with oral manifestations
- Behçet's disease is a rare systemic vasculitis characterised by recurrent oral ulcers, genital ulcers, and eye inflammation
- Systemic lupus erythematosus (SLE) is an autoimmune condition where oral ulcers are a recognised diagnostic criterion
If mouth ulcers are accompanied by abdominal symptoms, fatigue, joint pain, skin rashes, or eye problems, evaluation for these systemic conditions is essential.
7. Weakened Immune System
A compromised immune system, whether due to HIV/AIDS, chemotherapy, immunosuppressive medications (such as those used after organ transplantation or for autoimmune diseases), or chronic illnesses,s significantly increases susceptibility to oral ulcers and delays healing.
A lesser-known but clinically significant trigger is sodium lauryl sulphate (SLS), a foaming agent found in many commercial toothpastes. Research has shown that individuals who switch to SLS-free toothpaste often experience a notable reduction in the frequency of mouth ulcers. If you are prone to recurrent ulcers, this simple change is worth trying.
Symptoms of Recurring Mouth Ulcers
- Painful sores inside the mouth are often worse when eating, drinking, or speaking
- A burning or tingling sensation 24–48 hours before the ulcer appears
- Round or oval lesions with a white or yellow centre and a red, inflamed rim
- Swelling or tenderness in the surrounding tissue
- Heightened sensitivity to spicy, salty, or acidic foods
- In severe cases, swollen lymph nodes or mild fever
When Should You Be Concerned?
- An ulcer has not healed within 3 weeks
- The ulcer is unusually large, deep, or spreading
- New ulcers appear before previous ones have healed
- You experience systemic symptoms, such as weight loss, fatigue, or joint pain
- Ulcers recur with very high frequency, multiple times per month
- There is difficulty swallowing, speaking, or opening the mouth
Persistent, non-healing ulcers must be evaluated to exclude oral cancer, which can sometimes present as an ulcer-like lesion. Early diagnosis in such cases is critical for prognosis.
How Are Recurring Mouth Ulcers Diagnosed?
- Detailed clinical examination and full medical history review
- Blood tests: complete blood count, iron studies, B12, folate, zinc levels
- Autoimmune screen ANA, anti-dsDNA, and other markers if systemic disease is suspected
- Coeliac antibody testing tissue transglutaminase IgA (tTG-IgA)
- Allergy testing if specific food or contact triggers are suspected
- Biopsy for persistent, large, or atypical ulcers to exclude malignancy
Treatment Options for Frequent Mouth Ulcers
For mild, occasional ulcers, the following can provide symptomatic relief:
- Warm saltwater rinses gently cleanse the ulcer and reduce bacteria
- Honey is a natural antimicrobial agent with some evidence for ulcer healing
- Aloe vera gel applied topically to soothe inflammation
- Avoiding known food triggers during an active episode
- Staying well hydrated and eating soft, bland foods
- Antiseptic mouthwashes (e.g., chlorhexidine) reduce bacterial load
- Topical anaesthetic gels (e.g., benzocaine, lidocaine) provide temporary pain relief
- Protective pastes and gels form a barrier over the ulcer to shield it from irritation
Prescription Medical Treatment
When ulcers are frequent, severe, or related to an underlying condition, medical treatment is essential:
Vitamin and mineral supplementation correcting deficiencies is often highly effective
- Topical corticosteroids reduce local inflammation and speed healing
- Systemic corticosteroids for severe, widespread, or autoimmune-related ulcers
- Colchicine or dapsone is used in refractory cases or in conditions likeBehçet's disease
- Biologic therapies in complex inflammatory bowel disease or systemic autoimmune conditions
Preventing Mouth Ulcers: Daily Habits That Make a Difference
- Eat a balanced, nutrient-rich diet, prioritising leafy greens, legumes, whole grains, dairy, and lean protein to maintain adequate B12, iron, folate, and zinc levels
- Switch to an SLS-free toothpaste, particularly if you suffer from frequent recurrences
- Use a soft-bristled toothbrush, brush gently, and replace your brush every three months
- Identify and avoid personal food triggers, and maintain a diary to spot patterns
- Managing stress proactively, regular exercise, adequate sleep, and mindfulness practices reduce the inflammatory load
- Stay well hydrated; a dry mouth is more prone to tissue breakdown. Attending regular dental check-ups ensures that fitting appliances are used and that oral abnormalities are caught early.
- Do not ignore systemic symptoms. Early treatment of conditions like coeliac disease or inflammatory bowel disease reduces oral manifestations.s
Expert Care for Mouth Ulcers at Renova Hospitals
Final Thoughts
Medical Disclaimer
Category
- Joint Replacement
- Joint Replacement
- Joint Replacement
- Joint Replacement
- Joint Replacement
- Joint Replacement