Pancreatic cancer is one of the most dangerous cancers in India because it rarely shows symptoms in its early stages. The most important warning signs are jaundice (yellowing of skin or eyes), persistent upper abdominal or back pain, unexplained weight loss, and new-onset diabetes in adults over 50.
Key Takeaways:
- India’s high diabetes burden, widespread tobacco use (smoking and smokeless), and tropical pancreatitis increase overall risk.
- Nearly 95% of cases in India are diagnosed at advanced stages; early awareness and early action are critical.
- Incidence among Indian women is rising; awareness and timely evaluation are essential.
- New-onset diabetes after age 50 without typical risk factors should be medically evaluated.
- All forms of tobacco, cigarettes, gutka, pan, and chewing tobacco, significantly raise the risk. Quitting is the most powerful preventive step.
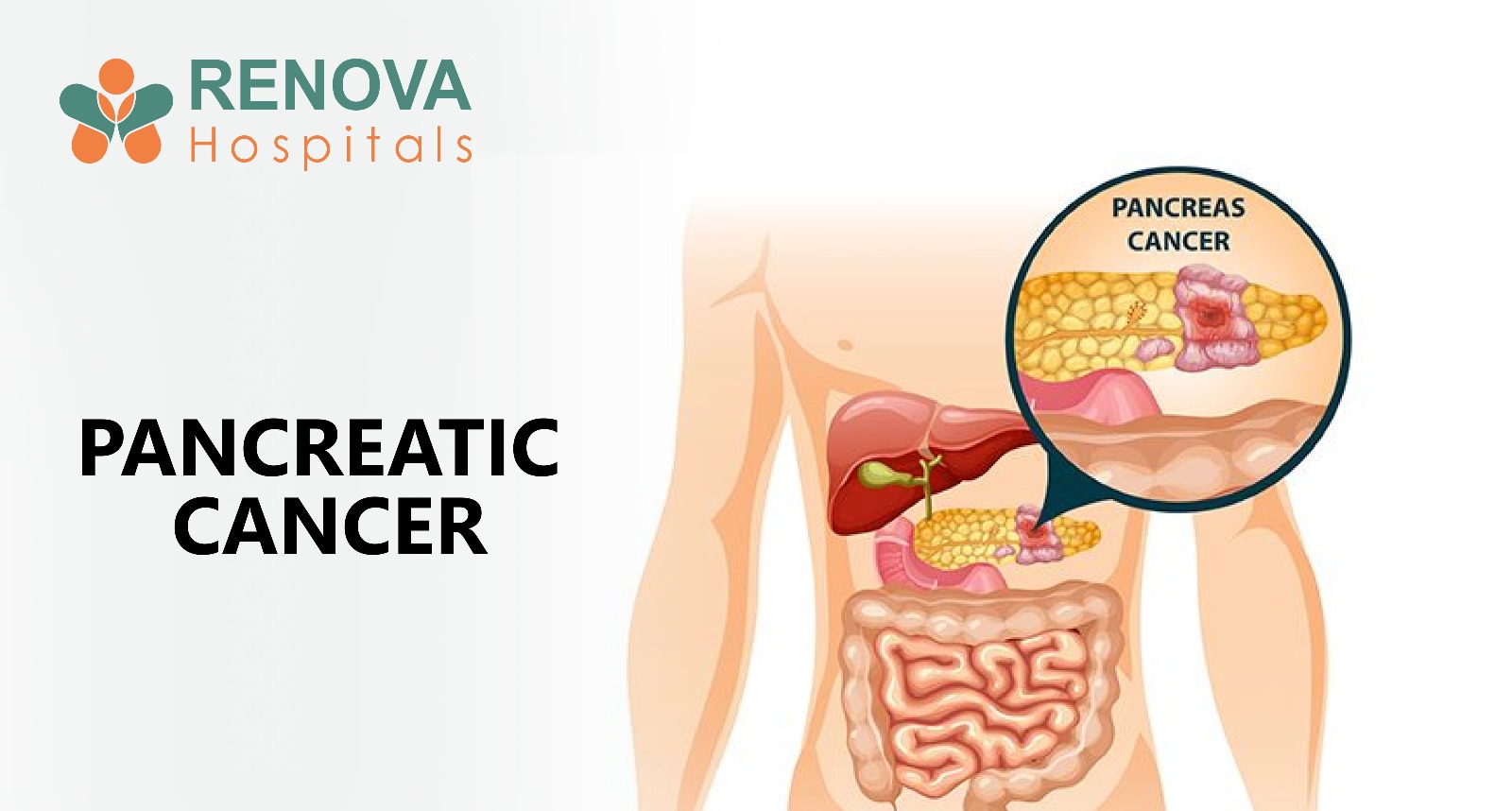
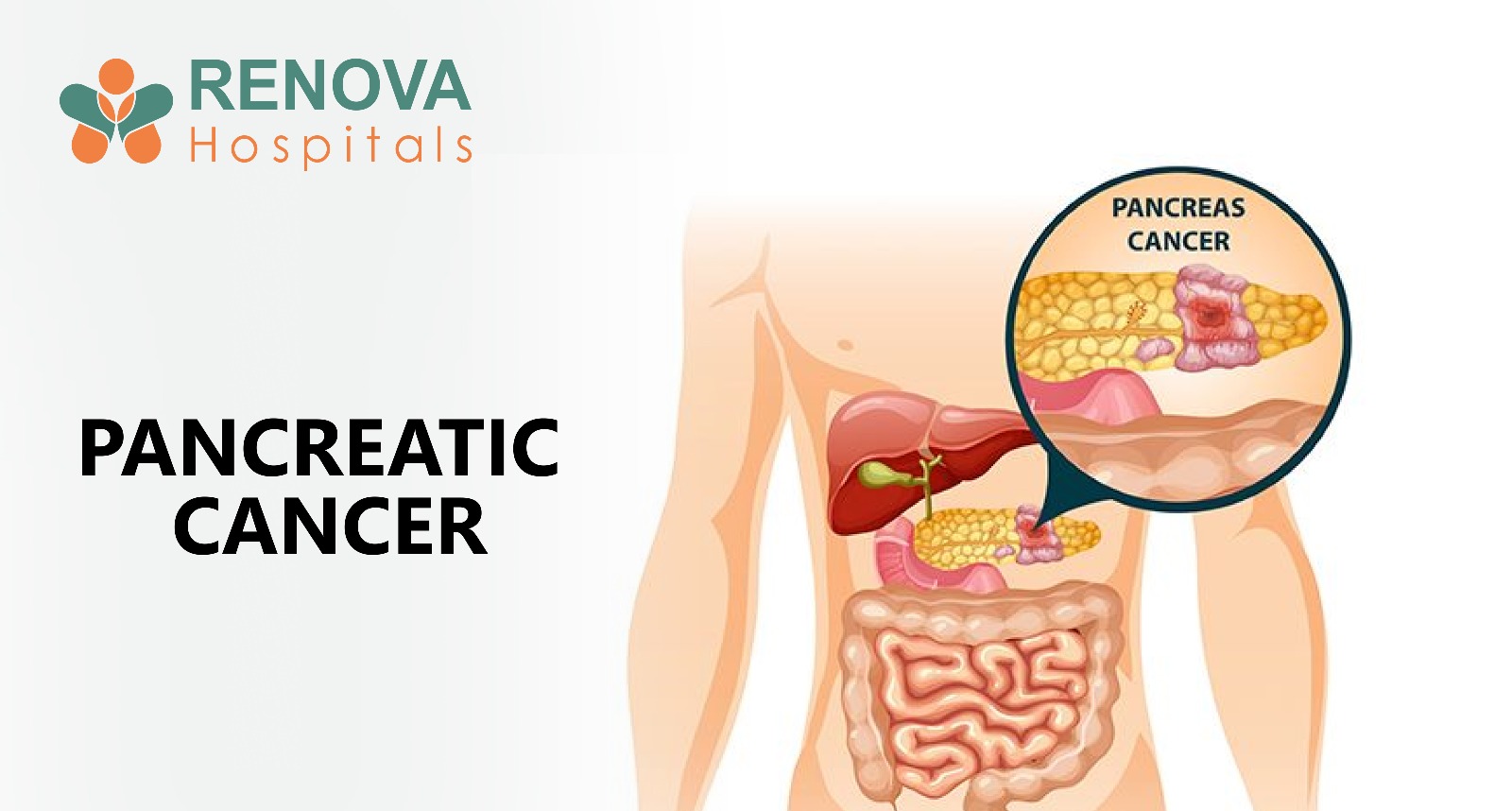
What is Pancreatic Cancer?
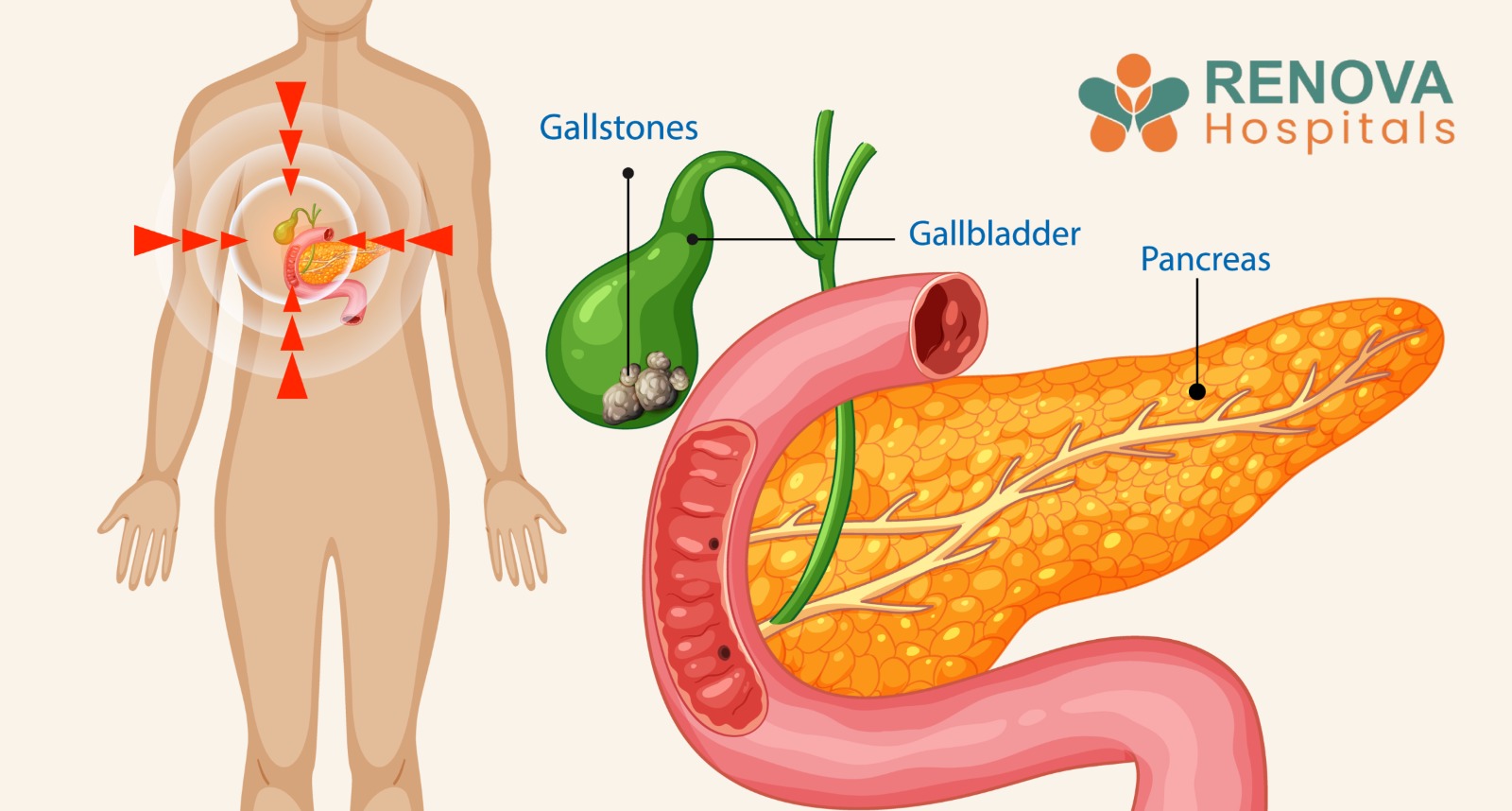
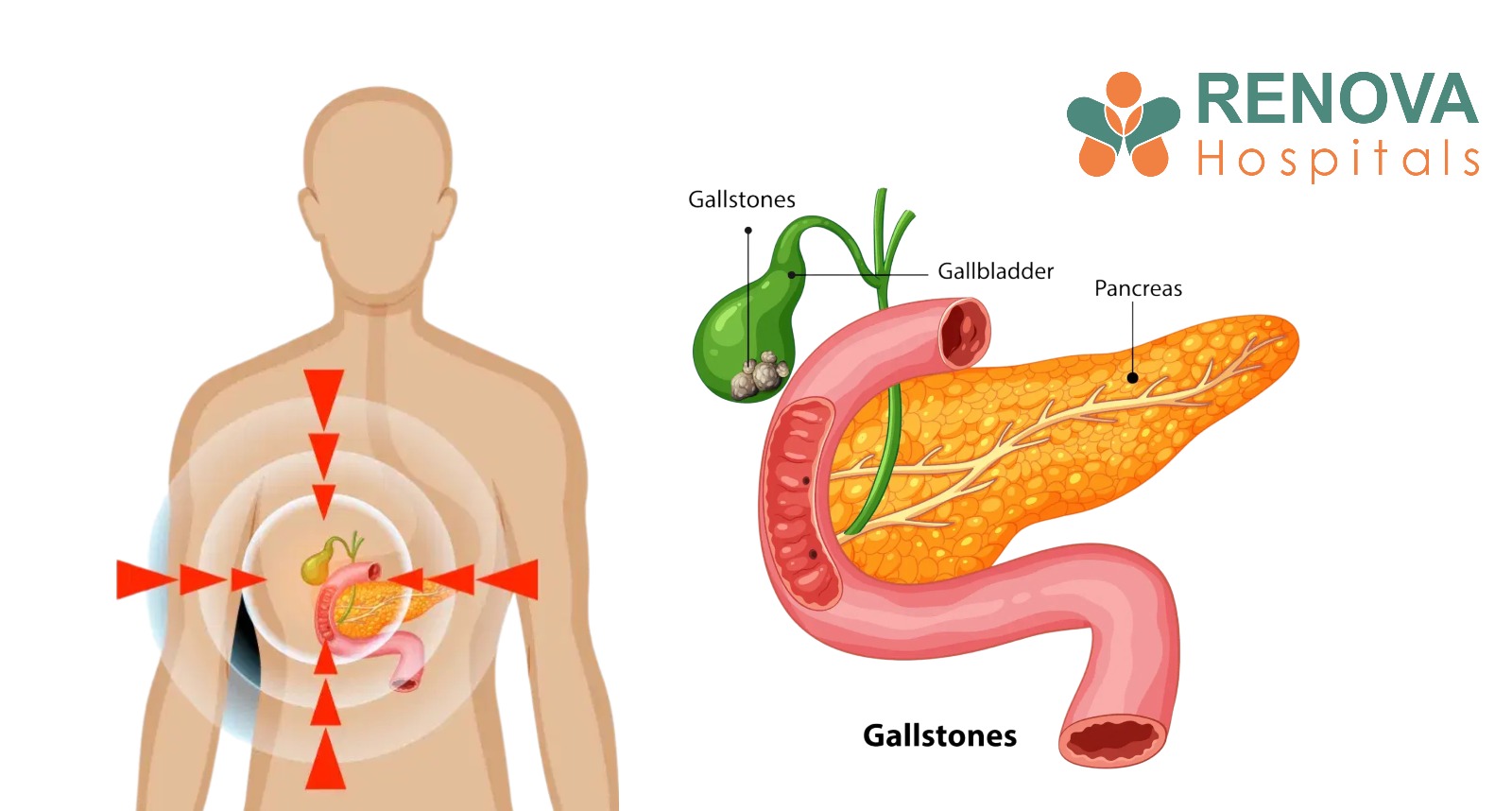
Pancreatic cancer begins in the tissues of the pancreas, an organ situated deep in the abdomen behind the stomach. The pancreas performs two critical roles: producing digestive enzymes that break down food, and secreting insulin to regulate blood sugar.
When cancer develops in the cells lining the pancreatic ducts, the most common form, known as pancreatic adenocarcinoma, tends to grow silently and aggressively before causing any obvious symptoms.
Key Statistics
India records approximately
10,860 new cases of pancreatic cancer annually, ranking it 24th in cancer incidence but 18th in cancer mortality in the country. This gap between incidence and mortality ranking reflects just how deadly the disease is, most patients in India are diagnosed at an advanced, inoperable stage.
Among the most alarming trends: female pancreatic cancer incidence in India is rising at
3.7% per year, one of the steepest increases of any country in the world. Cases are projected to increase steadily as India's population ages and lifestyle-related risk factors such as diabetes and obesity become more prevalent.
Why India Has a Unique Risk Profile
Several factors make the Indian context distinct from Western countries when it comes to pancreatic cancer risk.
1. India's Diabetes Epidemic
India carries one of the largest diabetes burdens in the world. Nearly 10% of adults are living with diabetes, and millions remain undiagnosed.
Long-standing type 2 diabetes increases the risk of pancreatic cancer by approximately
1.5 to 2 times. More importantly, new-onset diabetes after the age of 50, especially in individuals without obesity or a strong family history, may sometimes be an early sign of an underlying pancreatic tumour rather than routine metabolic disease.
Research shows that up to
80% of pancreatic cancer patients develop new-onset diabetes or impaired glucose tolerance around the time of diagnosis. In a country with such a massive diabetic population, this connection cannot be overlooked.
2. Tropical Pancreatitis - An India-Specific Risk Factor
Unlike Western countries, parts of India, particularly Kerala and Tamil Nadu, have a higher prevalence of tropical calcifying pancreatitis, a chronic inflammatory pancreatic disorder.
This condition carries an exceptionally high cancer risk. Studies have shown:
- A relative risk up to 100 times higher than the general population
- Pancreatic cancer develops at a much younger average age (around 45 years), compared to 70+ years in Western populations
This means Indian patients may develop pancreatic cancer decades earlier, making awareness and surveillance crucial.
3. High Tobacco Burden in Multiple Forms
India’s tobacco burden is not limited to cigarettes. Tobacco is consumed in multiple forms:
- Cigarettes
- Bidis
- Hookah
- Gutka and khaini
- Chewing tobacco and snuff
All forms significantly increase pancreatic cancer risk. Smoking alone raises the risk by nearly
75%, and the elevated risk can persist for up to 10 years even after quitting.
Smokeless tobacco, widely used across India, is equally dangerous and often underestimated.
4. Rising Obesity and Sedentary Lifestyles
Rapid urbanisation has changed dietary patterns and physical activity levels across Indian cities. Increasing consumption of ultra-processed foods, reduced physical movement, and high stress levels are contributing to:
- Abdominal obesity
- Insulin resistance
- Metabolic syndrome
South Asians are particularly prone to visceral (abdominal) fat, even at lower body weights. This metabolic pattern is strongly associated with increased cancer risk — including pancreatic cancer.
5. Late Diagnosis and Healthcare Access
Perhaps the most critical issue in India is delayed detection.
In many Western countries, around 15–20% of pancreatic cancers are detected at a stage where surgery is possible. In India, studies indicate that up to
95% of patients are diagnosed at advanced, non-localised stages.
Reasons include:
- Low awareness of early symptoms
- Mistaking abdominal pain and weight loss for acidity or gastritis
- Delayed referral to specialists
- Limited access to advanced imaging in semi-urban and rural regions
By the time patients seek specialist care, treatment options may already be limited.
What Are the Early Warning Signs of Pancreatic Cancer?
These symptoms apply universally but are especially important for Indians given the risk factors described above. Do not dismiss these as ordinary digestive problems, especially if they persist.
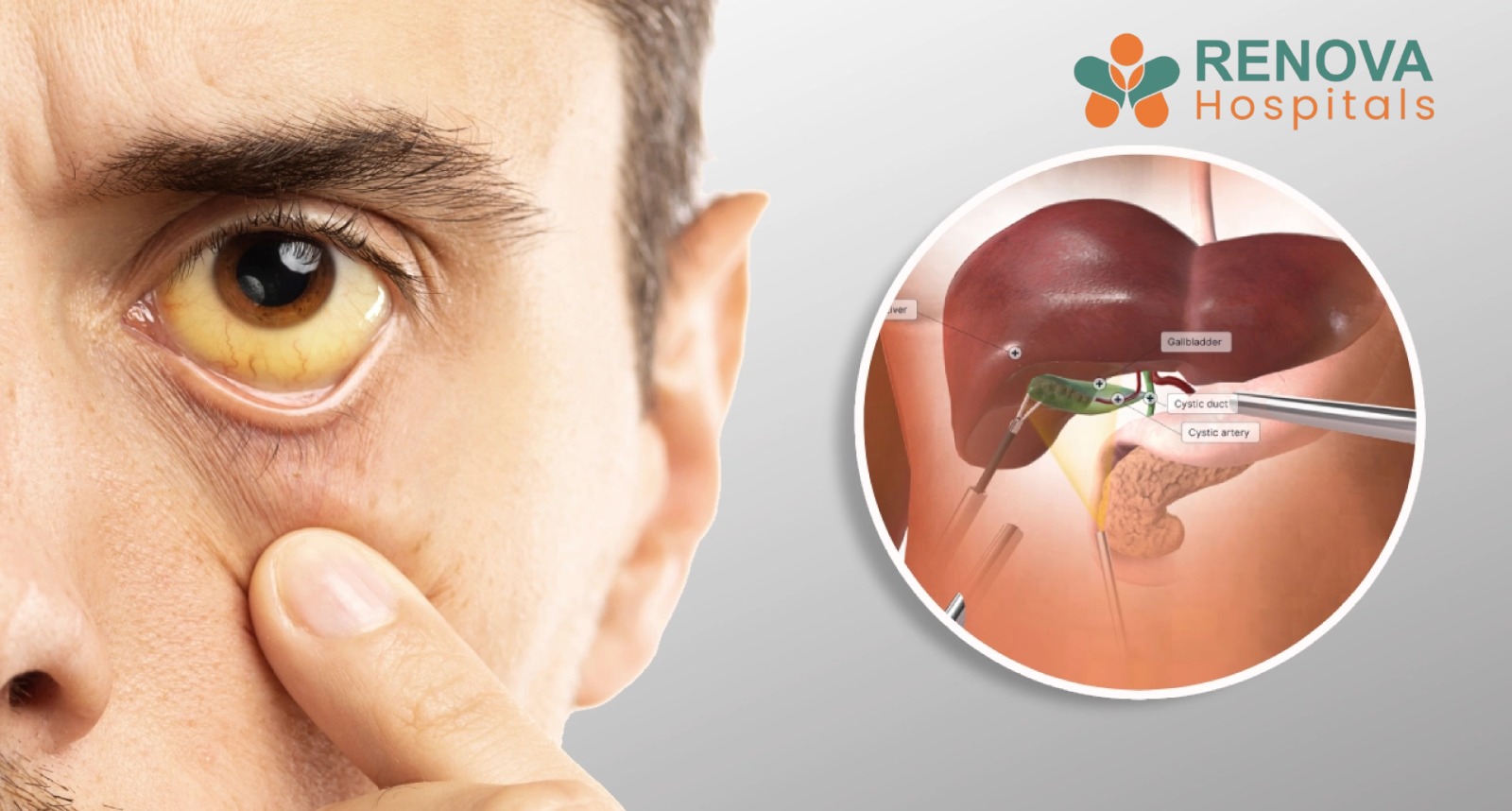
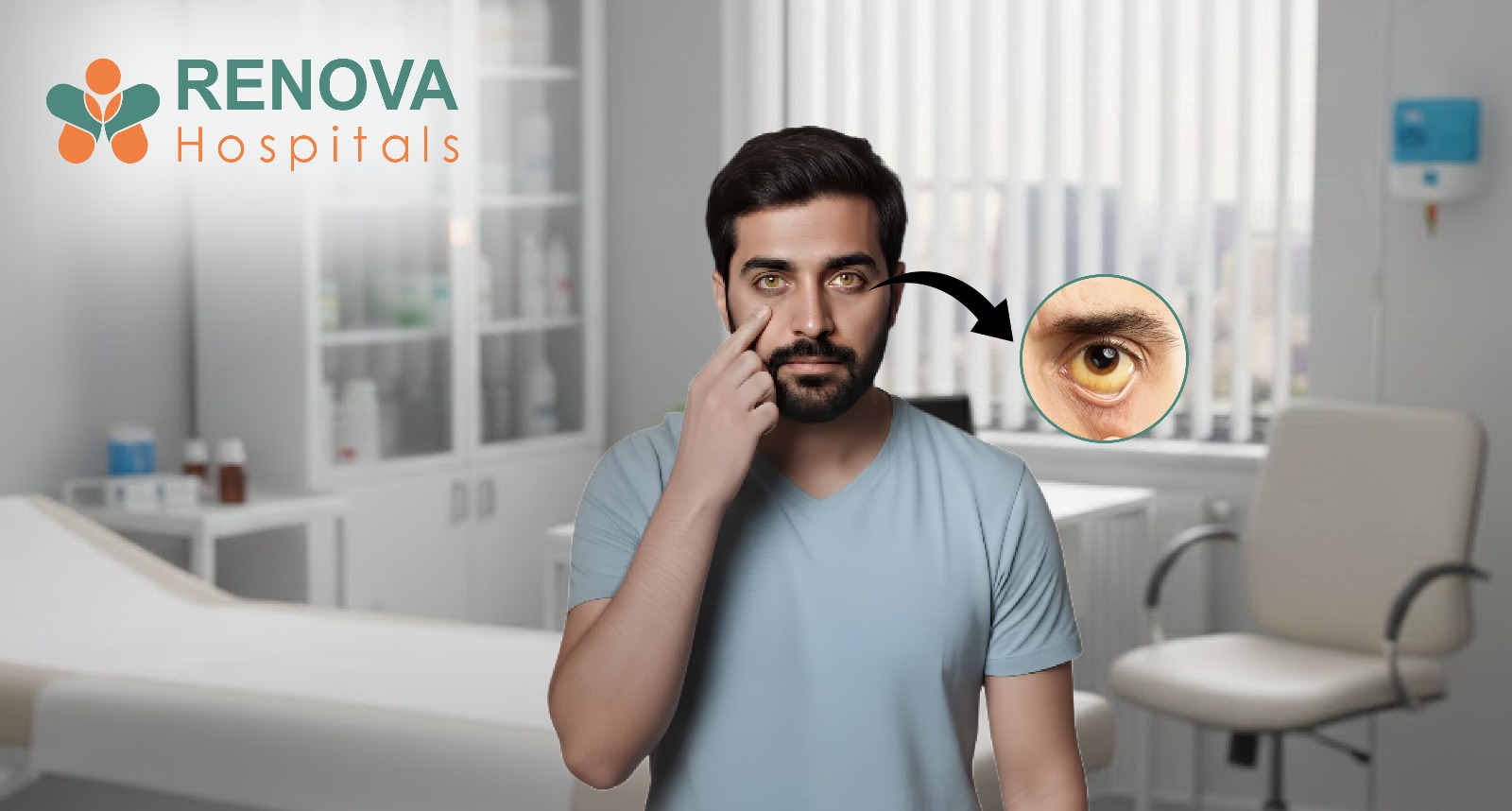
1. Jaundice - Yellowing of the Skin or Eyes
Jaundice occurs when a tumour in the head of the pancreas blocks the bile duct, causing bilirubin to build up in the blood. It is one of the most recognisable early signs and should never be ignored. Watch for:
• Yellowing of the whites of the eyes and skin
• Dark, tea-coloured urine
• Pale or clay-coloured stools
• Persistent itching of the skin without an obvious cause
2. Persistent Upper Abdominal or Back Pain
A dull, nagging pain in the upper abdomen that spreads to the middle of the back is one of the most common complaints. This pain is often mistaken for gastritis, acidity, or a back muscle problem. Key features include:
• Gets worse after eating
• Increases when lying flat on the back
• Temporarily eases when leaning forward
• Persists for more than 2 to 3 weeks despite standard treatment
3. Unexplained Weight Loss and Loss of Appetite
Because the pancreas helps digest food and absorb nutrients, a tumour disrupts this process significantly. Patients often notice:
• Rapid, unintentional weight loss, sometimes several kilograms in a few weeks
• Loss of appetite or feeling full after eating very little
• Persistent nausea or vomiting
• Extreme, unexplained fatigue
4. New-Onset or Suddenly Worsening Diabetes
This is a particularly important warning sign in the Indian context, given our very high diabetes burden. If an adult over 50 is suddenly diagnosed with diabetes without obvious risk factors, no strong family history, no major obesity, and no prior pre-diabetes or if a previously well-controlled diabetic suddenly loses control of their blood sugar for no clear reason, pancreatic cancer must be ruled out.
Research shows that new-onset diabetes can be one of the earliest detectable signals of pancreatic cancer.
When Should You See a Doctor?
Do not wait and watch. In India, where most patients are diagnosed at a very late stage, acting quickly on symptoms is the single most important step a patient can take. See a doctor or specialist immediately if you notice any of the following:
• Abdominal or back pain that has lasted more than 2 to 3 weeks
• Yellowing of the eyes or skin
• Unexplained weight loss, especially if rapid
• New diabetes after age 50 without obvious risk factors
• Sudden worsening of previously stable diabetes
• Persistent nausea, loss of appetite, or digestive discomfort
Ask your general physician to refer you to a
gastroenterologist or surgical oncologist if symptoms persist. Do not accept a diagnosis of 'acidity' or '
gastritis' without investigation if symptoms do not resolve promptly.
How Is Pancreatic Cancer Diagnosed?
The diagnostic pathway in India often involves multiple steps, and there can be significant delays at each stage. Understanding the process helps patients advocate for themselves.
Step 1 - Clinical Evaluation
Your doctor will review symptoms, duration of pain, risk factors, family history, diabetes status, and all forms of tobacco use. A focused physical examination follows.
Step 2 - Blood Tests
Tests include liver function tests, blood sugar levels, and tumour markers like CA 19-9 and CEA. Elevated CA 19-9 with symptoms requires urgent imaging, though it cannot confirm cancer alone.
Step 3 - Imaging
An abdominal ultrasound is usually the first test. If suspicion arises, a contrast-enhanced CT scan is essential to assess tumour size and operability. MRI and Endoscopic Ultrasound (EUS) provide a more detailed evaluation at specialised centres.
Step 4 - Endoscopic Procedures
ERCP may be performed to relieve bile duct blockage in jaundiced patients. EUS helps visualise the tumour closely and guides the biopsy.
Step 5 - Biopsy
A tissue sample, typically obtained through EUS-guided fine needle aspiration, confirms the diagnosis. Treatment should begin only after pathological confirmation.
Do Not Wait for Severe Symptoms, Act Early
Pancreatic cancer may be silent in its early stages, but India's unique risk factors make awareness even more critical for us than in many other parts of the world.
Whether you use tobacco in any form, live with diabetes, have a history of pancreatitis, or simply have persistent digestive symptoms that are not resolving, do not wait.
Speak to a specialist. Ask for investigations. The difference between an early and late diagnosis in this disease can be the difference between life and death.
Our
oncology team at Renova Hospitals is here to help. Early consultation, the right tests, and timely treatment give you the best chance of a good outcome.