By Renova Hospitals
February 24, 2026
Oral Cancer in India: Causes, Early Signs, Survival & How to Prevent It
Key Takeaways
- India accounts for over one-third of global oral cancer cases, with more than 70,000 new diagnoses annually, making it a significant public health concern.
- Tobacco use (smoked and smokeless) is the leading cause of oral cancer, responsible for up to 75–90% of cases.
- The overall 5-year survival rate in India is approximately 37%, but early-stage oral cancer has survival rates close to 70%.
- Late diagnosis is the biggest reason for poor outcomes, especially in rural areas with limited access to screening.
- Gutka, areca nut, and alcohol significantly increase oral cancer risk, particularly when used together.
- Oral cancer is largely preventable and highly treatable when detected early, making awareness and regular screening critical.
Despite advances in oncology, the 5-year survival rate of oral cancer in India remains approximately 37%, mainly due to late-stage detection.
What Is Oral Cancer?
Oral cancer refers to malignant tumours that develop in the oral cavity, including:
- Tongue
- Floor of the mouth
- Gums
- Buccal mucosa (inner cheeks)
- Hard palate
- Lips
Why Oral Cancer Is Increasing in India
- High tobacco consumption (smoked and smokeless)
- Widespread use of gutka, pan masala, khaini, and areca nut
- Alcohol consumption
- Low awareness of early symptoms
- Limited rural screening access
- Delayed medical consultation
- Overall 5-year survival rate: 37.2%
- Rural survival rate: ~34%
- Urban survival rate: ~48%
- Localised cancer survival: ~70%
- Distant metastasis survival: ~9%
Major Causes of Oral Cancer
1. Tobacco and Oral Cancer (Primary Risk Factor)
Forms associated with high risk:
- Cigarette smoking
- Bidi smoking
- Cigar and pipe use
- Smokeless tobacco (gutka, khaini, snuff)
- Betel quid with tobacco
- Smokers have a 5–6 times higher risk
- Heavy smokers may have a 10–27 times higher risk
- 75–90% of oral cancers are attributable to tobacco
- Risk decreases by about 50% within 3–5 years of quitting
- Oral submucous fibrosis (a potentially malignant disorder)
- Buccal mucosa cancer
- Early-age oral cancer cases
- Heavy alcohol consumption significantly increases risk.
- Combined heavy smoking + heavy drinking may increase the risk up to 38 times in men.
- Alcohol weakens the lining of the mouth, making it easier for harmful substances to damage cells.
4. HPV and Oral Cancer
- HPV 16
- HPV 18
- Base of tongue cancer
- Oropharyngeal cancer
Oral cancers linked to HPV often respond better to treatment, but early detection is still essential. In India, HPV plays a contributory but minor role compared to tobacco-related cancers.
- Fruits and vegetables
- Vitamin C
- Vitamin E
- Beta-carotene
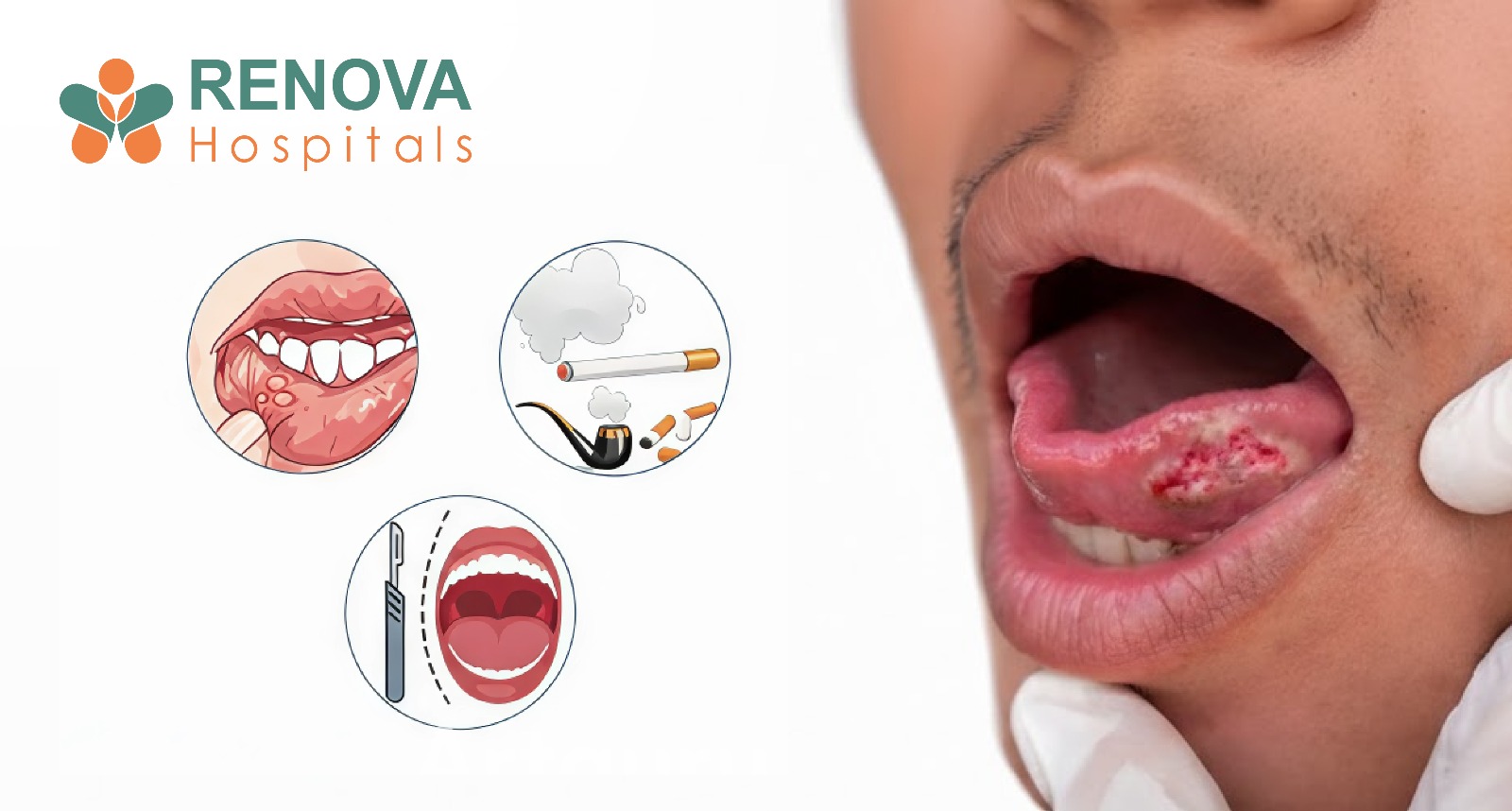
Early Signs and Symptoms of Oral Cancer
Early Symptoms (Critical for Early Detection)
- Persistent white patch (leukoplakia)
- Red patch (erythroplakia)
- Non-healing ulcer lasting more than 2 weeks
- Unexplained oral bleeding
- Sudden tooth mobility
- Persistent hoarseness
- Difficulty swallowing (dysphagia)
- Jaw stiffness (trismus)
- Neck swelling (enlarged lymph nodes)
- Chronic ear pain
- Persistent oral pain
- Airway obstruction
How Oral Cancer Is Diagnosed
1. Clinical Examination
- Detailed tobacco and alcohol history
- Visual inspection of the oral cavity
- Palpation of cervical lymph nodes
- Tongue protraction examination
- Incisional biopsy
- Excisional biopsy
- Fine needle aspiration (for suspicious lymph nodes)
- CT scan (bone invasion, nodal metastasis)
- MRI (soft tissue assessment)
- PET-CT (advanced staging and distant metastasis evaluation)
TNM Staging of Oral Cancer
- Stage I typically involves small tumours (≤2 cm) without lymph node spread.
- Stage II includes tumours measuring 2-4 cm without nodal involvement.
- Stage III usually involves larger tumours or a single lymph node.
- Stage IV indicates advanced disease with multiple lymph nodes or distant metastasis.
Early-stage cancers have significantly better survival outcomes compared to advanced stages.
Survival Rate of Oral Cancer in India
An extensive population-based cohort study of over 14,000 patients revealed:
- Overall 5-year survival: 37.2%
- Localised disease: ~70% survival
- Regional spread: ~37%
- Distant metastasis: <10%
- Age ≥65 years: 1.7 times higher mortality risk
- Rural residence: 30% higher risk of death
Field Cancerization: Risk of Second Primary Cancer
Even after treatment, patients remain at risk of developing another cancer because the mouth lining may have been exposed to harmful substances for years.
- 16–36% risk of second primary tumours
- 3–5% annual risk of new malignancy
- Most second cancers occur within 3 years
Prevention of Oral Cancer
Primary Prevention
- Complete cessation of all tobacco products
- Avoid gutka, pan masala, and areca nut
- Limit alcohol consumption
- Eat at least 5 servings of fruits and vegetables daily
- Use lip sunscreen for outdoor workers
- Promote HPV vaccination awareness
- Annual oral cancer screening after age 40
- Monthly self-examination of the oral cavity
- Immediate evaluation of persistent lesions
- Multidisciplinary cancer care
- Complete treatment adherence
- Lifelong follow-up and surveillance
Medical Disclaimer
Early evaluation and diagnosis significantly improve treatment outcomes. In case of urgent or severe symptoms, seek immediate medical attention. Always consult an oncologist or oral health specialist for personalised medical advice and treatment planning.
Category
- Joint Replacement
- Joint Replacement
- Joint Replacement
- Joint Replacement
- Joint Replacement
- Joint Replacement