By Renova Hospitals
February 23, 2026
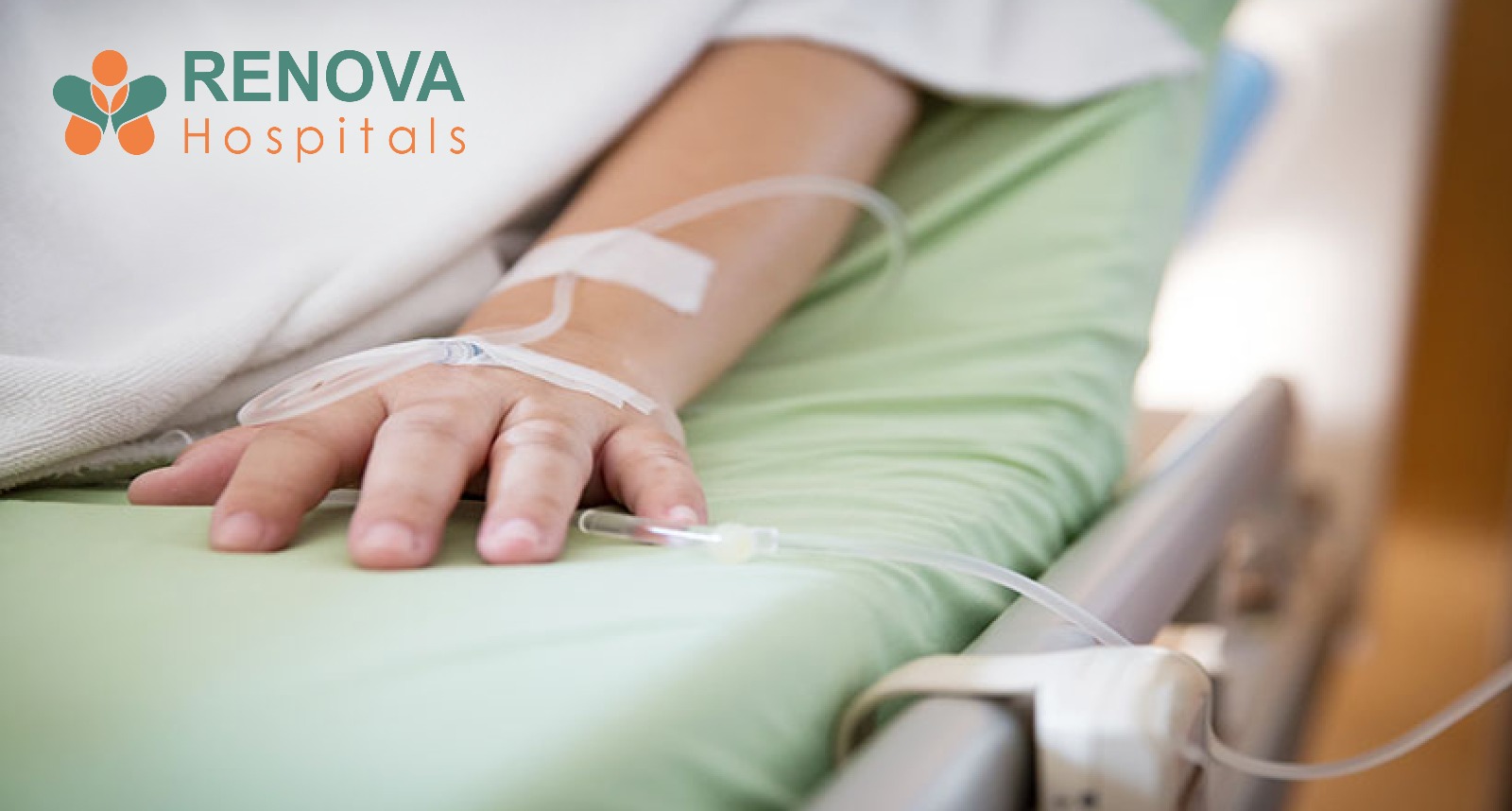
Childhood Cancer in India: Why Early Diagnosis Can Save More Lives
- In India, childhood cancer makes up about 4% of all cancer cases, with nearly 52,000 children diagnosed each year.
- Globally, nearly 400,000 children (0–14 years) are diagnosed with cancer each year.
- In high-income countries, survival rates are often above 80–90%, but in many low- and middle-income countries, outcomes are still much poorer.
- Strengthening early detection, referral systems, pediatric oncology infrastructure, and survivorship care is essential.
- Global efforts, such as the WHO’s childhood cancer initiative, aim to improve survival rates to at least 60% worldwide by 2030.
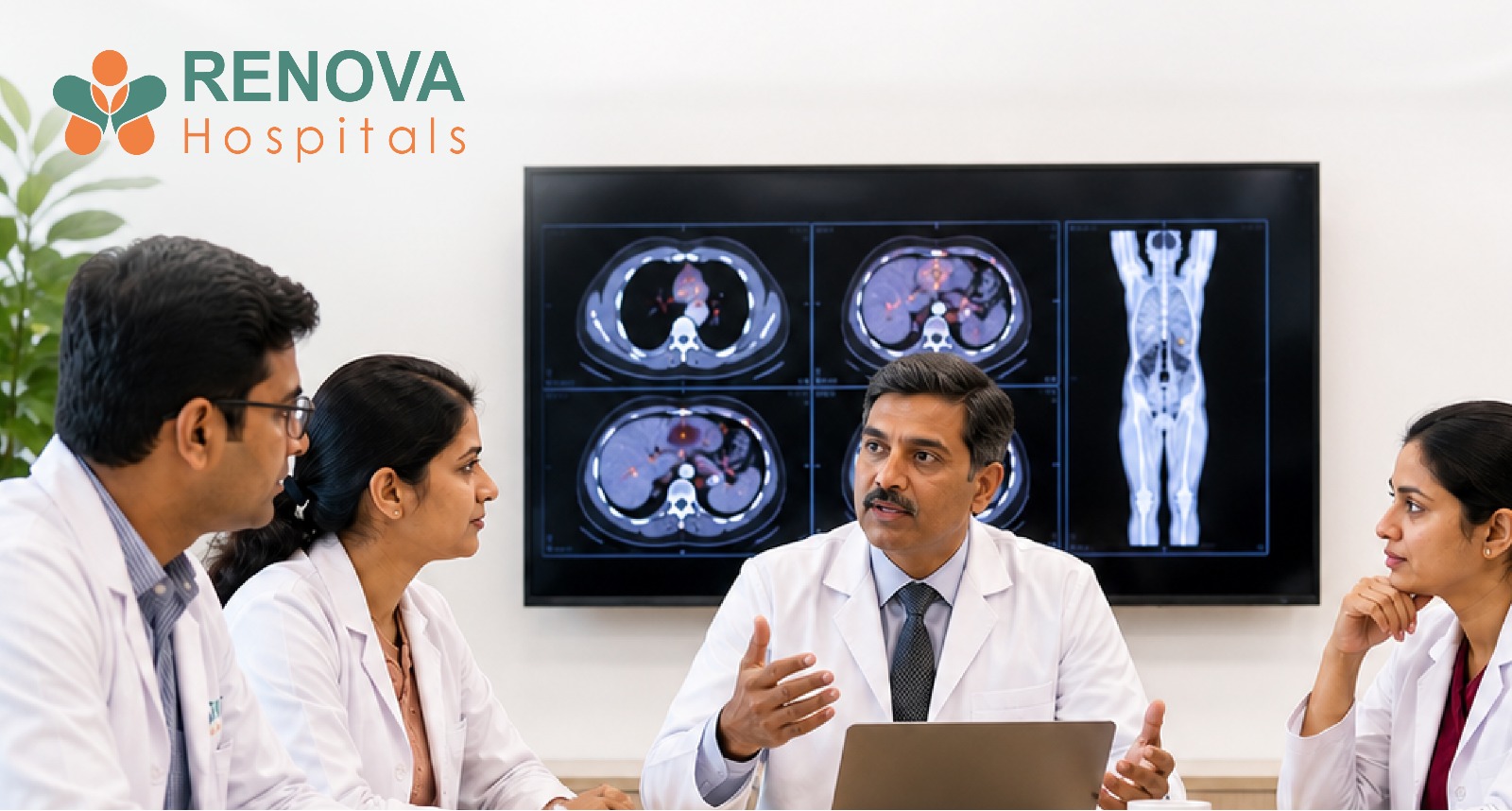
Understanding Childhood Cancer: A Global Perspective
Childhood cancer is an important global health issue that affects families across the world. According to the World Health Organisation, approximately 400,000 children aged 0–14 years are diagnosed with cancer each year worldwide.
While more than 85% of children survive in high-income countries, survival can fall to 20–30% in lower-income regions, often because the disease is diagnosed late or treatment is difficult to access.
- Leukaemia (most common globally)
- Brain and central nervous system (CNS) tumours
- Lymphomas
- Neuroblastoma
- Wilms tumor
- Bone cancers such as osteosarcoma and Ewing sarcoma
Key Indian Data Highlights:
- An estimated 52,000 cases annually (0–14 years)
- Approximately 13,700 childhood cancer deaths were reported in 2010
- Incidence rates have been rising over the past decade.
- Regional disparities in diagnosis and reporting
The rising burden is partly due to:
- Improved diagnostic capacity
- Increased cancer awareness
- Population growth
- Better registry reporting
- Limited awareness of early warning signs
- Symptoms mimicking common infections
- Delays in referral to specialist centres
- Diagnostic infrastructure gaps in rural areas
- Average treatment cost: ₹1–7 lakh per case
- Around 70% of expenses are out-of-pocket.
- Non-medical costs (travel, accommodation, food) add to the hardship.
- Treatment abandonment rates in some regions have been reported as high as 40–90%
- Delayed treatment initiation
- Missed follow-ups
- Travel-related financial strain
- Pediatric oncologists
- Hematologists
- Oncology nurses
- Radiologists
- Social workers
- Nutrition specialists
Workforce shortages and uneven distribution of facilities remain significant barriers.
Government Initiatives and Global Collaborations
- The CURE-ALL approach emphasises early diagnosis and comprehensive care
- Strengthening of cancer registries
- Standardisation of treatment protocols
- Improved medicine procurement
Treatment options for childhood cancer have improved significantly in recent years.
- Molecular risk stratification in acute lymphoblastic leukaemia (ALL)
- Targeted therapies based on genetic mutations
- Precision radiotherapy to reduce organ damage
- CAR-T cell therapy
- Reduced-intensity treatment protocols for low-risk cases
- Improved early detection
- Affordable access to essential medicines
- Strengthened referral systems
- Expanded pediatric oncology training programs
- Treatment is more effective
- Complications are fewer
- Long-term survival increases
- Treatment costs may be lower.
- Cardiac complications
- Endocrine disorders
- Secondary cancers
- Cognitive challenges
- Lifelong monitoring
- Psychosocial counseling
- Nutritional support
- Rehabilitation services
Improving childhood cancer care in India will require coordinated efforts at multiple levels:
- Strengthen cancer registries and data accuracy
- Expand regional pediatric oncology centres.
- Improve financial protection mechanisms.
- Invest in workforce training.
- Integrate mental health and supportive care.
- Enhance community education and early referral.
No child should miss out on life-saving treatment because of where they live, financial hardship, or lack of information.
Category
- Joint Replacement
- Joint Replacement
- Joint Replacement
- Joint Replacement
- Joint Replacement
- Joint Replacement