Key Takeaways:
- Every injury is unique - Orthopedic care tailored to your biology, lifestyle, and goals consistently produces better outcomes than one-size-fits-all treatment.
- Individualised rehabilitation reduces re-injury risk by up to 51% - Recovery programs designed around a patient’s specific injury and daily demands help prevent recurring pain.
- Regenerative therapies like PRP and stem cell treatments address the root cause - These therapies focus on tissue repair rather than simply masking symptoms, and may delay or reduce the need for surgery in selected patients.
- Many orthopedic injuries are predictable - Preventive screening can identify biomechanical weaknesses long before they result in ligament tears or chronic joint damage.
- Modern orthopedic care goes beyond pain control - True recovery restores strength, corrects movement patterns, and prevents patients from returning with the same injury later.
Most people rarely think about their joints until something suddenly goes wrong. It might be a sharp pop during a run, a shoulder that refuses to stop aching, or a knee that swells after standing for hours. When patients finally visit an orthopedic clinic, they often receive a standard treatment plan that looks almost identical for everyone.
That approach is part of the problem. When treatment is generic, many patients find themselves returning months later with the same issue, frustrated that the pain never truly resolved.
Fortunately, orthopedic medicine is evolving. Modern care is increasingly personalised, focusing on the individual patient rather than the diagnosis alone. Understanding what personalised orthopedic care involves can help explain why outcomes are improving dramatically.
Moving Beyond Standardised Orthopedic Treatment
Musculoskeletal disorders affect more than 1.71 billion people worldwide, according to the
Bone and Joint Initiative USA, making them the leading cause of disability globally. Despite this enormous burden, orthopedic treatment for many years followed a fairly predictable formula: rest, medication to control inflammation, and surgery when necessary.
However, two patients with the same diagnosis can have very different recovery needs. A personalised orthopedic care approach takes several factors into account:
- Age and activity demands - A 28-year-old athlete will recover differently from a 55-year-old professional who spends most of the day at a desk.
- Tissue health and healing potential - Nutrition, sleep quality, and underlying medical conditions influence recovery speed.
- Biomechanical patterns - The way a person moves often explains why an injury occurred in the first place.
- Personal goals - Returning to competitive sport requires a very different rehabilitation strategy than returning to routine daily activity.
Custom Rehabilitation: Where Real Recovery Happens
Many people imagine rehabilitation as a simple list of exercises printed on a sheet of paper. In reality, structured rehabilitation at a specialised centre is one of the most powerful tools in orthopedic recovery - provided the program is tailored to the patient.
A 2021 review published in the Journal of
Orthopaedic & Sports Physical Therapy reported that individualised rehabilitation programs reduced re-injury rates by as much as 51% compared with standardised protocols.
Modern orthopedic rehabilitation now includes several advanced components:
- Neuromuscular retraining - Restoring the communication between the brain and muscles that injury often disrupts.
- Sport- or job-specific movement training - Exercises designed to reflect the real physical demands of a patient’s daily life.
- Progressive loading strategies - Carefully increasing stress on healing tissues at the correct stage of recovery.
- Strength and conditioning programs - Building resilience and joint stability beyond the pre-injury baseline.
- Structured return-to-activity planning - Using measurable milestones instead of guesswork.
In a comprehensive orthopedic and spine care model, rehabilitation does not end when pain disappears. It concludes only when the patient has regained strength, stability, and confidence in their movement.
Regenerative Medicine: Treating the Source, Not Just the Symptoms
One of the most exciting developments in orthopedics today is the rise of regenerative medicine. Instead of simply reducing pain, these therapies aim to activate the body’s own healing processes to repair damaged tissue.
Platelet-Rich Plasma (PRP)
PRP therapy involves drawing a small sample of the patient’s blood, concentrating the platelets, and injecting them directly into the injured area. Platelets contain growth factors that support tissue repair and regeneration.
Because the injection uses the patient’s own biological material, the risk of adverse reactions is extremely low.
PRP is commonly used to treat:
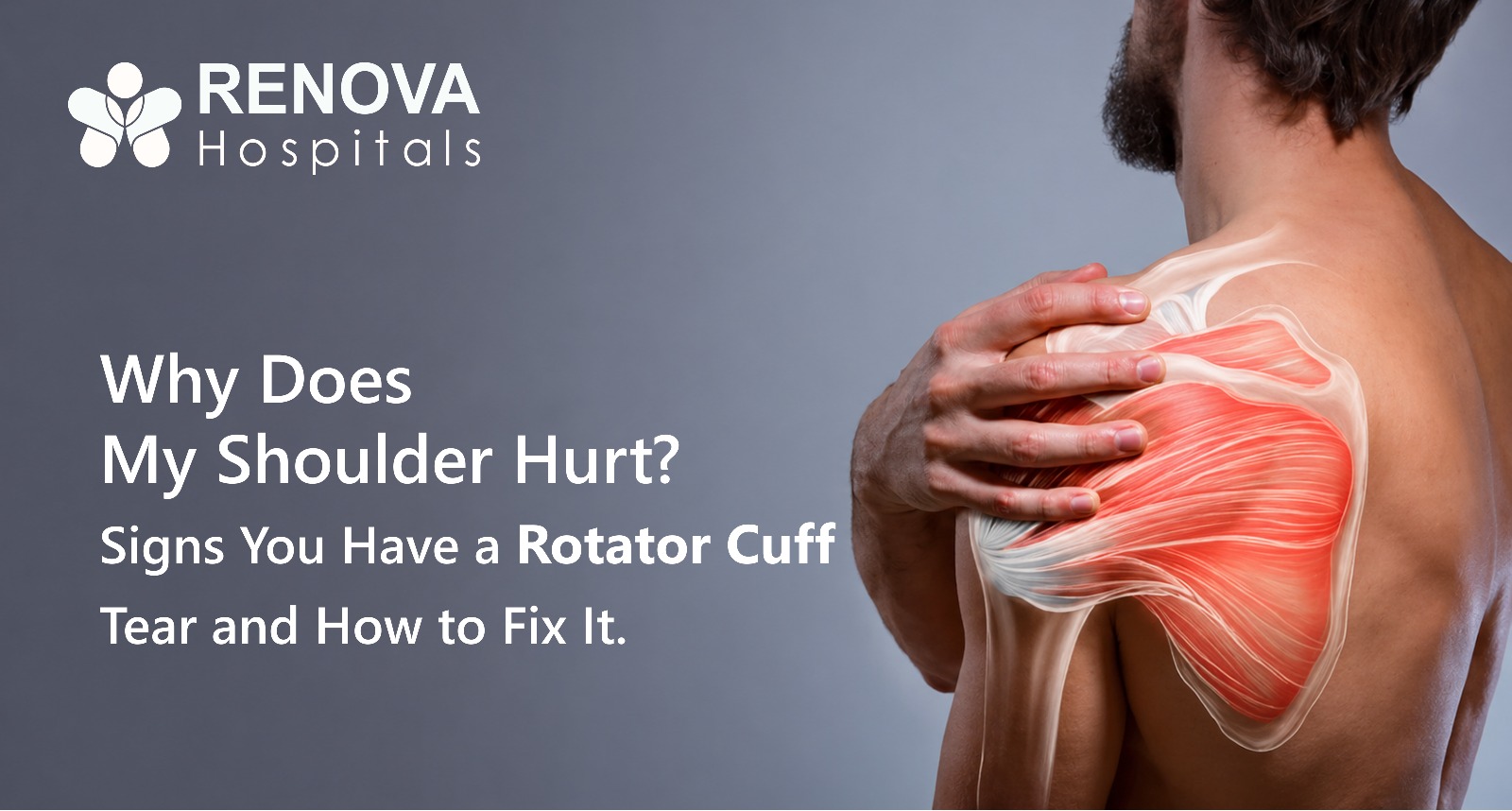
- Tennis elbow and rotator cuff injuries
- Chronic tendon inflammation
- Early osteoarthritis
A
meta-analysis published in the American Journal of Sports Medicine found that PRP injections produced significantly better outcomes than corticosteroid injections for chronic tendon injuries, with benefits lasting up to a year.
Stem Cell Therapy
Stem cell-based regenerative therapies represent another major advancement. Stem cells can develop into specialised cells such as cartilage, bone, or tendon tissue, making them particularly useful for treating degenerative joint conditions.
Important considerations include:
- Best suited for moderate joint degeneration, rather than advanced disease
- May delay or reduce the need for surgical procedures in selected patients
- The global orthopedic stem cell therapy market is projected to grow at over 10% CAGR through 2030, reflecting increasing adoption and clinical interest
It is important to note that regenerative treatments are not suitable for every patient. Careful evaluation by an orthopedic specialist is essential to determine whether these therapies are appropriate.
Preventive Injury Screening: Stopping Injuries Before They Occur
An often overlooked fact in orthopaedics is that many serious injuries can actually be predicted. Biomechanical warning signs frequently appear months or even years before a ligament tear or chronic joint condition develops.
Common early indicators include:
- Muscle imbalances
- Reduced joint mobility
- Asymmetrical movement patterns
- Postural adaptations caused by prolonged desk work or repetitive sports activity
Preventive injury screening aims to identify these issues early.
A comprehensive assessment typically evaluates:
- Joint mobility and flexibility
- Muscle strength and left-right asymmetry
- Movement mechanics during functional activities
- Postural alignment
- The history of previous injuries is one of the strongest predictors of future problems
The results of preventive programs are impressive. Research published in the British Journal of Sports Medicine found that athletes who underwent movement screening and targeted corrective training reduced ACL injury rates by up to 70%.
Importantly, these screenings are not limited to professional athletes. Office workers, physically demanding labourers, and older adults can all benefit from identifying movement weaknesses before they lead to injury.
The Bigger Picture: Precision Orthopaedics Is the Future
Orthopaedic medicine has always focused on restoring mobility and helping people return to their daily lives. What has changed is the level of precision with which this can now be achieved.
Global
projections suggest that more than 1 billion people may be affected by musculoskeletal disorders by 2050, highlighting the growing need for advanced orthopedic care.
For patients, the most important question to ask an orthopedic specialist is no longer simply “What is wrong?” but rather:
“What treatment strategy is specifically designed for me?"