By Renova Hospitals
March 31, 2026
Antibiotic Resistance: Why It’s Becoming a Serious Health Concern Today
Introduction: A Crisis We Can’t Ignore Anymore
When action is delayed, bacteria can change in ways that make antibiotics ineffective, making infections harder to treat and increasing risks.
Globally, antibiotic resistance is already responsible for millions of deaths every year. If timely action is not taken, it could become the leading cause of death in the coming decades. This is why antibiotic resistance is often referred to as a “silent pandemic.”
Key Takeaways
- Antibiotic resistance occurs when bacteria stop responding to medicines, making infections harder to treat
- Misuse and overuse of antibiotics are the main drivers of resistance worldwide.
- India faces a higher risk due to easy access, high infection rates, and a lack of awareness.
- Resistant infections can lead to longer illness, higher costs, and serious complications.s
- Even routine medical procedures become risky when antibiotics are no longer effective.
- Responsible antibiotic use, hygiene, and early medical consultation can help protect both individual and public health. and their communities, making a real difference in the fight against antibiotic resistance.
What Is Antibiotic Resistance?
Antibiotic resistance happens when bacteria develop the ability to survive exposure to antibiotics that would normally kill them.
- Medicines stop working
- Infections become harder to treat
- Patients may need stronger and more expensive drugs
Why Antibiotic Resistance Is a Major Healthcare Threat
1. Increasing Deaths and Disease Burden
- Easy access to antibiotics without a prescription
- High population density
- Increased infection rates
- Lack of awareness about proper antibiotic use
- Surgeries
- Organ transplants
- Cancer chemotherapy
- Intensive care treatments
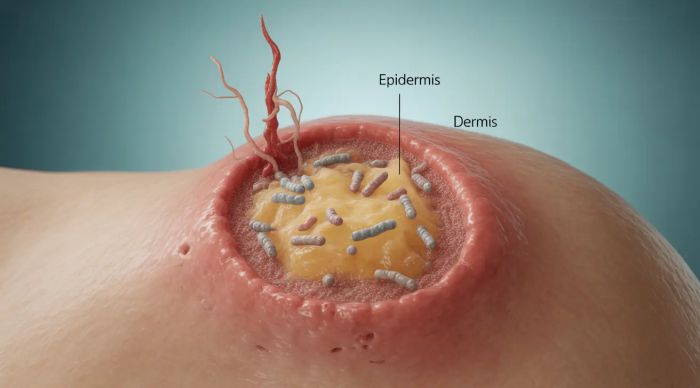
How Antibiotic Resistance Develops
Bacteria are highly adaptable organisms. They can develop resistance through different mechanisms:
Key Mechanisms
- Preventing the drug from entering the cell
- Changing the target that the antibiotic attacks
- Producing enzymes that destroy the drug
- Pumping the drug out of the cell
Common “Superbugs” You Should Know
Certain bacteria have developed resistance to multiple antibiotics and are often called superbugs.
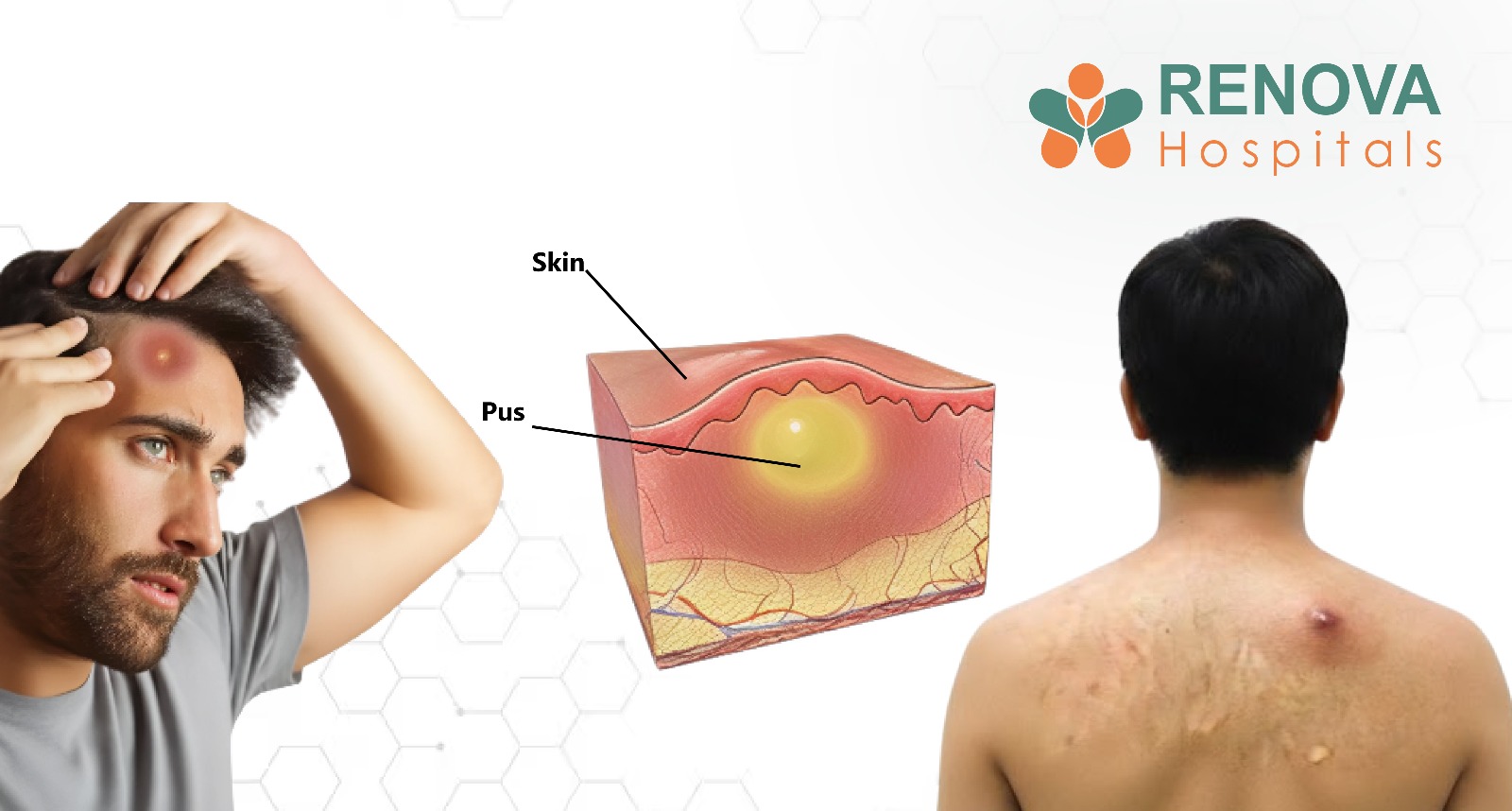
- MRSA – causes severe skin and bloodstream infections
- CRE – highly resistant bacteria with high mortality rates
- ESBL-producing bacteria are resistant to many commonly used antibiotics
- MDR-TB – drug-resistant tuberculosis
What Causes Antibiotic Resistance?
- Taking antibiotics for viral infections like the cold or flu
- Self-medication without consulting a doctor
- Stopping treatment midway
- Wrong medicine
- Incorrect dosage
- Improper duration
- Poor hand hygiene
- Overcrowded healthcare settings
- Inadequate infection control practices
Impact on Patients and Healthcare
For Patients
- Longer recovery times
- Increased risk of complications
- More severe illness
- Higher treatment costs
- Increased patient load
- Longer hospital stays
- Higher ICU demand
- Increased healthcare costs
- Financial burden due to expensive treatments
- Loss of income due to prolonged illness
- Emotional stress
How Can We Prevent Antibiotic Resistance?
The good news is that antibiotic resistance can be slowed down with the right actions.
- Take antibiotics only when prescribed
- Follow the full course of treatment
- Never share medicines
How Renova Hospitals Supports Safe Antibiotic Use
- Accurate diagnosis before prescribing antibiotics
- Evidence-based treatment protocols
- Strict infection control measures
- Patient education on proper medication use
Conclusion: Take Action Before It’s Too Late
Antibiotic resistance is not just a medical issue; it is a global responsibility. If we continue to misuse antibiotics, we risk losing one of the most powerful tools in modern medicine.
- Use antibiotics wisely
- Follow medical advice
- Spread awareness
This content is for informational purposes only and should not be considered medical advice. Always consult a qualified healthcare professional for diagnosis and treatment.
Category
- Joint Replacement
- Joint Replacement
- Joint Replacement
- Joint Replacement
- Joint Replacement
- Joint Replacement